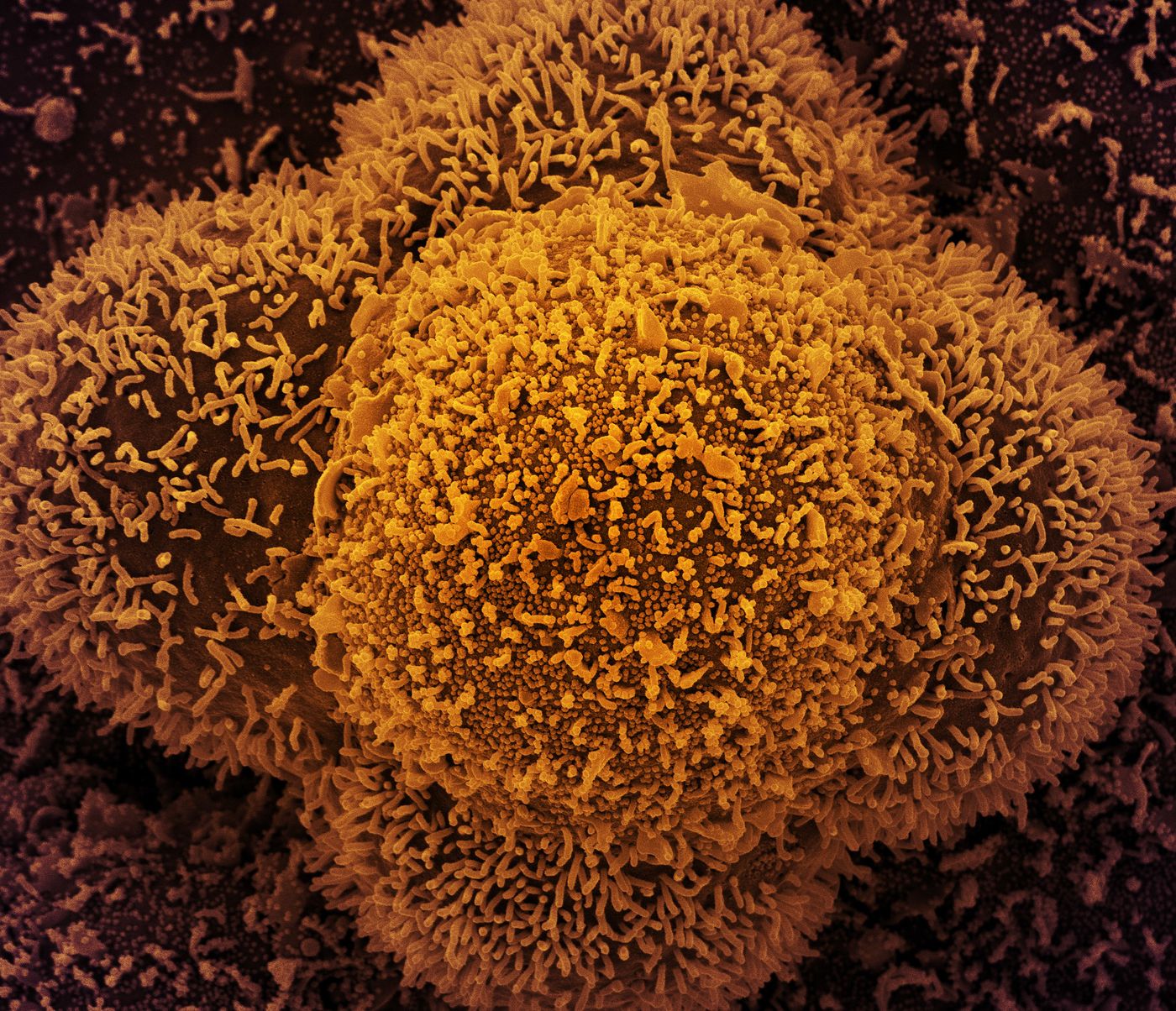
Cell Atlas Helps Explain the Deadly Nature of SARS-CoV-2
For over a year now, scientists and clinicians have been trying to understand why SARS-CoV-2 causes such deadly infections in some people. Recent research has investigated the lungs of individuals that died from COVID-19, and the work has revealed more about what the virus does. In people that died from the virus, there was a devastating trifecta of uncontrolled inflammation, direct destruction and faulty regeneration in lung cells that are involved in the exchange of gases (oxygen and carbon dioxide), and rapid scarring. This work can also help researchers learn about the causes of potential long-term respiratory effects from the scarring.
"It's a devastating disease, but the picture we're getting of the COVID-19 lung is the first step towards identifying potential targets and therapies that disrupt some of the disease's vicious circuits. In particular, targeting cells responsible for pulmonary fibrosis early on could possibly prevent or ameliorate long-term complications in survivors of severe COVID-19," said Benjamin Izar, M.D., Ph.D., assistant professor of medicine at Columbia University Irving Medical Center (CUIMC).
This work involved over 40 researchers from institutions including CUIMC, Harvard, and MIT, who published two reports in Nature. The effort to characterize cells at the single-cell level has created a lung atlas of COVID-infected lung cells.
"A normal lung will have many of the same cells we find in COVID, but in different proportions and different activation states," explained Izar. "In order to understand how COVID-19 is different compared to both control lungs and other forms of infectious pneumonias, we needed to look at thousands of cells, one by one."
This study utilized lung tissue from 19 people who died of COVID-19, and their tissues and cells were compared to lung cell samples from patients with different respiratory illnesses. In COVID patients, the lungs were loaded with immune cells called macrophages. These cells are important front-line defenders against pathogens; they can destroy invaders directly and can help regulate the immune response. But the immune system has to be carefully controlled, and things can go awry when these macrophages are dealing with SARS-CoV-2.
"In COVID-19, we see expansion and uncontrolled activation of macrophages, including alveolar macrophages and monocyte-derived macrophages," Izar said. "They are completely out of balance and allow inflammation to ramp up unchecked. This results in a vicious cycle where more immune cells come in causing even more inflammation, which ultimately damages the lung tissue."
The macrophages were found to produce high levels of an inflammatory cytokine called IL-1ß. "Unlike other cytokines such as IL-6, which appears to be universally prevalent in various pneumonias, IL-1ß production in macrophages is more pronounced in COVID-19 compared to other viral or bacterial lung infections. That's important because drugs exist that tamp down the effects of IL-1ß," Izar said. There are clinical trials underway that are testing some of these drugs in COVID-19 patients.
Our tissues can also do repair work. In a normal infection in which a virus has damaged lung cells, once the pathogen is cleared, the cells can regenerate. But SARS-CoV-2 stops the process; it can ruin alveolar epithelial cells (that exchange gases), and devastate the ability of other cells to repair the damage. Cells that are capable of repair are still present, but they get trapped in a non-restorative state due to inflammation, and they cannot replace the mature cells.
"Among others, IL-1ß appears to be a culprit in inducing and maintaining this intermediate cell state, thereby linking inflammation and impaired lung regeneration in COVID-19," said Izar. "This suggests that in addition to reducing inflammation, targeting IL-1ß may help take the brakes off cells required for lung repair."
The work also identified a set of cells called pathological fibroblasts that quickly cause scarring in SARS-CoV-2-infected lungs. Scar tissue builds up in the lungs in a process called fibrosis, and there's less space in the organ for normal cells to do their work.
An algorithm was used to try to find drug targets for some of the molecules that are involved in these processes.
"This analysis predicted that inhibition of STAT signaling could alleviate some of the deleterious effects caused by pathological fibroblasts," Izar said. "Our hope is that by sharing this analysis and massive data resource, other researchers and drug companies can begin to test and expand on these ideas and find treatments to not only treat critically ill patients, but also reduce complications in people who survive severe COVID-19."
Sources: AAAS/Eurekalert! via Columbia University Irving Medical Center, Nature Melms et al 2021, Nature Delorey et al 2021