Small Clinical Trial Suggests New Edible Cholera Vaccine Is Safe
According to the World Health Organization, there have been six cholera pandemics since the bacterial pathogen emerged from the Ganges river delta sometime in the 19th century. Cholera is caused by the water-contaminating bacterium Vibrio cholerae. It's thought to cause from 1 to 4 million cases of cholera every year. While some of them cause no symptoms and many resolve on their own, the diarrheal disease has also caused from 21,000 to 143,000 deaths annually worldwide.
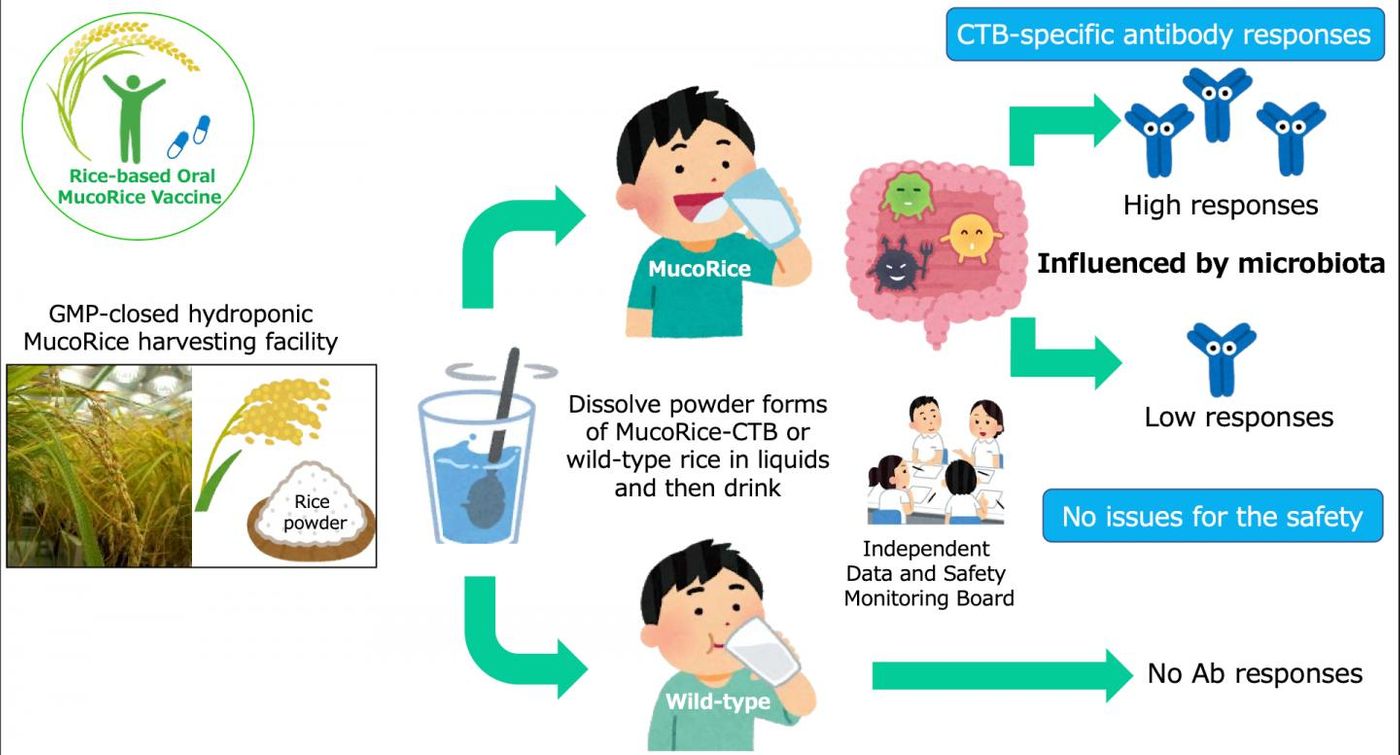
Currently available cholera vaccines have cold-storage requirements and are made from weakened cholera cells. But scientists have now created what may be a better vaccine for cholera; it's made from ground up grains of genetically modified rice and is stable at room temperature. These co-called MucoRice have been engineered to produce a non-toxic portion of cholera toxin B (CTB). The rice don't have to be processed either; the immune-stimulating antigens it makes are protected from stomach acids by the rice grains, which don't have to be refrigerated.
A human trial has been conducted; the results suggested that the vaccine does not cause serious side effects and does trigger a robust immune response. The findings from the Phase 1 trial of MucoRice-CTB have been reported in The Lancet Microbe.
"I'm very optimistic for the future of our MucoRice-CTB vaccine, especially because of the dose escalation results. Participants responded to the vaccine at the low, medium and high doses, with the largest immune response at the highest dose," explained project leader Professor Hiroshi Kiyono, D.D.S., Ph.D. of the Institute of Medical Science at the University of Tokyo.
In the small trial, volunteers were given either a placebo or the vaccine in a series of four doses two weeks apart. Three levels were tested: 3, 6, or 18 milligrams. When the researchers assayed for antibodies in the volunteers two and four months after the final dose, they found that volunteers that developed antibodies generated both IgAs and IgGs that were specific to CTB. Higher doses were more likely to result in the production of CTB antibodies.
MucoRice-CTB can use the mucous membranes of the intestine to gain entry into the body, which mimics some natural infections.
"The beautiful part of our vaccine is that it wisely uses the body's mucosal immune system through the gut for the induction of antigen-specific antibodies," said Kiyono.
When the mucosal immune system is stimulated it tends to trigger IgG and IgA production while injected vaccines often cause the production of IgG antibodies, but not IgAs.
In this trial, eleven of 30 people that had gotten the vaccine did not produce measurable antibodies. "When we saw those data about the eleven low and nonresponders, we thought maybe gut microflora have an influence on the outcome of the immune response," noted Kiyono.
The researchers assessed the gut microbiomes of the study volunteers. "In simplified terms, high responders had more diversified microflora, and in the low-responder group, diversity was much narrower," said Kiyono. "It's all speculation right now, but maybe higher microflora diversity creates a better situation for strong immune response against oral vaccine."
Vaccines are usually created in developed nations. When they are deployed in developing regions, they are less effective. Researchers have suggested that this is because of the mucosa-immune link; when individuals with chronic intestinal inflammation caused by poor sanitation get vaccinated, the vaccines don't trigger a strong immune response.
"Probably for every vaccination right now, even injected vaccines, we should think of the immune status of the individual based on the condition of their microflora," suggested Kiyono. More research will be necessary before the relationship between the mucosa and the MucoRice edible vaccine can be deciphered.
This study was very small, so the researchers know a lot more work will be needed to confirm the findings from this report. They are now planning additional clinical trials.
Sources: AAAS/Eurekalert! via University of Tokyo, The Lancet Microbe