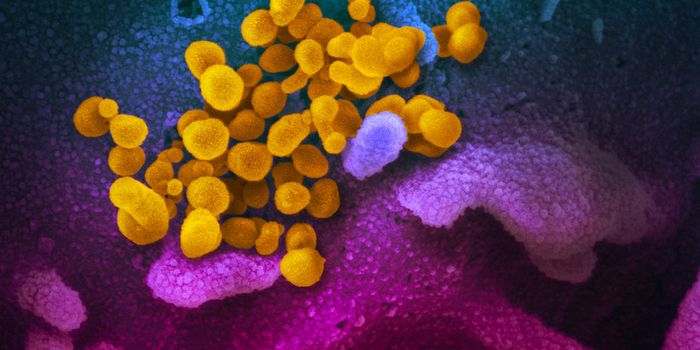
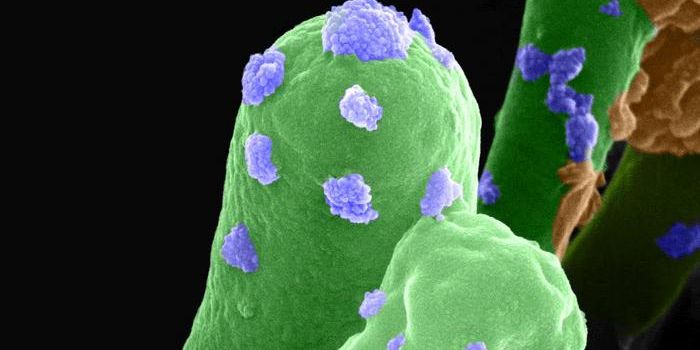
Malaria Vaccine Developed by Using Genetic Modifications
Malaria has been a global health problem for ages; it comes from a parasite that is over 130 million years old and is referenced as early as 2700 BC. Researchers may have found some real success in combating the problem at its root, rather than through symptom treatment. A clinical trial using human subjects showed that a new vaccine was safe to use and tolerated by people, and it was effective in inducing the necessary immune response. The work, performed by researchers at the Center for Infectious Disease Research (CIDR) and Fred Hutchinson Cancer Research Center, was reported in Science Translational Medicine. It's discussed in part of the following video, starting at around the second minute.
The researchers utilized a malaria parasite that had been weakened by removing three genes that are required for the pathogenicity of the parasite. The so-called genetically attenuated parasites, GAPs, are unable to reproduce in the human liver. The immune system still builds up an immunity to malaria through the parasite because they remain alive. This is the first use of a genetically attenuated parasite, instead of attenuation by other means, and it has produced success where other methods have failed.
"This most recent publication builds on our previous work," said the GAP project leader, Sebastian Mikolajczak, Ph.D., a CIDR Principal Scientist. "We had already good indicators in preclinical studies that this new 'triple knock-out' GAP (GAP3KO), which has three genes removed, is completely attenuated. The clinical study now shows that the GAP3KO vaccine is completely attenuated in humans and also shows that even after only a single administration, it elicits a robust immune response against the malaria parasite. Together these findings are critical milestones for malaria vaccine development.”
"This report is a major advance in malaria vaccine development by providing the first evidence that genetically attenuated Plasmodium falciparum parasites are safe and immunogenic in humans," commented Robert Seder, M.D., Chief of Cellular Immunology at the Vaccine Research Center of the National Institutes of Health, who was not involved in this work. "Future studies demonstrating protective efficacy will be the next critical milestone for continued development of this promising vaccine approach.”
The GAP3KO project was completed at the CIDR Human Challenge Center, a part of the Seattle Malaria Clinical Trials Center, an inter-institutional collaboration that works to fight malaria through drug and vaccine development.
"We are very fortunate to have the human malaria challenge model to take the critical next step evaluating the efficacy of GAP3KO in preventing malaria in people," said Fred Hutch scientist James Kublin, M.D., M.P.H., the Medical Director of the Seattle MCTC. "The Hutch is looking forward to bringing its expertise in clinical trial design and management to the next stage of tests for this vaccine. The collaborations we have with CIDR and other nearby institutions is what makes Seattle a world leader in the malaria vaccine development and the human challenge model."
Malaria causes over 200 million infections, killing almost half a million people in 2015 alone. This new candidate could be a major step forward for regions plagued by the parasite.
Sources: AAAS/Eurekalert! via Fearey Group, Malaria.com, Science Translational Medicine