Intrinsic resistance - they're born with it
Not all cases of antibiotic resistance stem from mutations - many bacteria are intrinsically resistant. This type of resistance is conferred by traits that are common to an entire species of bacteria - having an outer membrane, for example. All of these traits that confer intrinsic antibiotic resistance are referred to as the “intrinsic resistome” (everyone loves an “ome.” Am I right?)
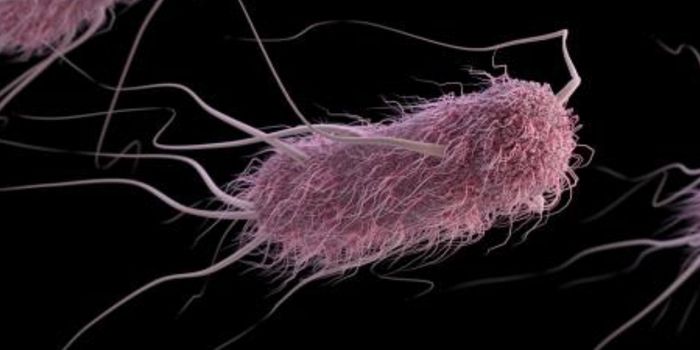
For starters, the outer membrane of Gram-negative bacteria is a major intrinsic resistance determinant because it does not allow large molecules to pass through it. The outer membrane contains tightly packed fatty acid chains that decrease membrane fluidity - this decreases the permeability, effectively excluding molecules that are larger that 500 Da.
Another example of intrinsic resistance occurs with vancomycin. This drug interferes with cell wall assembly, but it is only active against Gram-positive cells because vancomycin can’t cross the outer membrane of Gram-negative bacteria. (Clearly, it pays to be Gram-negative.)
The outer membrane is so impermeable, in fact, that these bacteria have to use channels called porins to regulate the influx and efflux of nutrients. These porins are still pretty impermeable to antibiotics because they regulate the passage of molecules based on charge, hydrophobicity, and size.
Gram-positive bacteria, on the other hand, are bound by a cytoplasmic membrane surrounded by a layer of peptidoglycan. This layer of peptidoglycan actually allows rather larger molecules to pass through, as does the cytoplasmic membrane. These factors make the Gram-positive bacteria intrinsically susceptible to antibiotics.
For example, daptomycin readily kills Gram-positive bacteria, but it doesn’t kill Gram-negative bacteria. This is because anionic phospholipids in the cytoplasmic membrane help daptomycin enter the cell - Gram-positive bacteria have a lot of these, Gram-negatives don’t.
Environmental microbes - particularly soil-dwelling bacteria - possess intrinsic resistance traits that actually predate the use of modern antibiotics. It is highly unlikely that these environmental microbes would pose a health threat, but there is evidence that they can transfer their resistance determinants to human pathogens.
Many soil-dwelling bacteria produce antibiotics. In order to protect themselves, however, they also produce resistance elements - it’s the genes for these elements that could potentially be transferred to other bacteria, including human pathogens. Not to mention, other soil bacteria that are exposed to antibiotics can acquire resistance mutations. Likewise, these genetic elements could be passed on to other bacteria.
In fact, researchers performed a large-scale screen of soil bacteria, and every strain they tested was resistant to multiple antibiotics! These and other data show that humans aren’t totally to blame for antibiotic resistance.
So, what can we do to combat intrinsic resistance? Researchers seem to agree that the outer membrane and efflux pumps are the most logical resistance mechanisms to target.
Polymyxins and colistin are cyclic cationic lipopeptides that have been used to disrupt the outer membrane of Gram-negative bacteria. Unfortunately, these drugs are associated with toxicity, and bacteria have already become resistant.
When it comes to blocking efflux pumps, phenyl-arginine-𝛃-naphthylamide is a competitive inhibitor of the MexAB-OprM system in P. aeruginosa. When efflux pumps are blocked, the concentration of antibiotic increases inside the cell because the drug can’t be pumped out.
Georgina Cox and Gerard Wright, researchers at McMaster University, sum it up well. “The effectiveness of front-line clinical treatments continues to dwindle in the face of emerging [multidrug resistant] bacteria. To prevent a global human threat from occurring, it is paramount that novel therapeutic strategies and new antibacterial agents are developed. As the intrinsic resistance of Gram-negative bacteria dramatically limits therapeutic options, the intrinsic resistome of bacteria represents an attractive therapeutic target to allow the identification of antibiotic adjuvants that rejuvenate the activity of existing antibiotics.”
Sources: International Journal of Medical Microbiology, Science, Nature, Nature Reviews Microbiology