Bacteria may be to Blame for Diseases of Chronic Inflammation
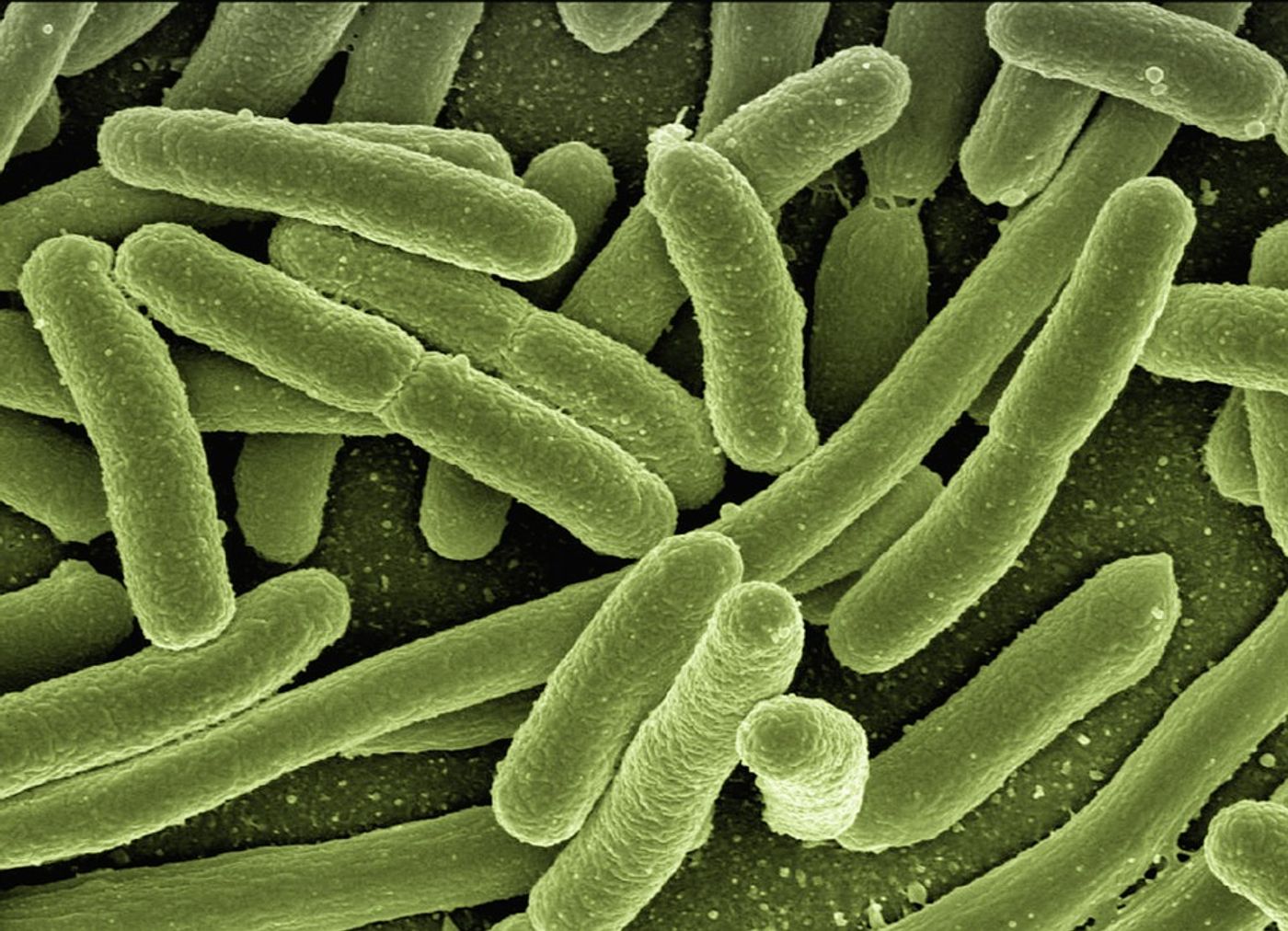
We live among trillions of different kinds of bacteria, many of which are harmless, while some can even be beneficial to us. But some microbes are responsible for deadly infection, and new research suggests they may also be to blame for some serious diseases that are not thought to be associated with bacteria. Scientists are now hypothesizing that microbes may cause inflammation that leads to chronic conditions like rheumatoid arthritis, type 2 diabetes, Parkinson’s and Alzheimer's diseases.
Professors Resia Pretorius of Stellenbosch University (SU) in South Africa and Professor Douglas B. Kell of The University of Manchester in the United Kingdom have previously found evidence that these disorders have microbial origins. These conditions are not like bacterial infections.
"If the bacteria were active, or replicating, as in the case of infectious diseases, we would have known all about that," explained Kell. "But the microbes are not replicating, they're mainly actually dormant."
Since the bacteria are dormant, they are thought to be absent from human blood; there is an assumption that our blood is sterile. However, when blood iron levels are high, such as in inflammatory diseases, this dormant bacteria can be awakened. Research has suggested that given the right conditions, microbes can begin to replicate again and secrete lipopolysaccharides (LPS), which compounds the inflammation.
Some are of the opinion that inflammation could be considered the basis for disease, and it is a typical feature of many chronic disorders. Pretorius and Kell, who discuss their work in the video above, have found that one cause of inflammation, abnormal blood clotting, can be caused by parts of bacterial cell walls, like LPS and Lipoteichoic acid (LTA).
Disorders of blood clotting are called coagulopathies, and are common features of inflammatory diseases. Scientists have found they lead to the amyloid formation, which causes structural problems in blood clotting proteins. That may be causing cell death or neurodegeneration.
Individuals with disease have abnormal fibrin fibers in blood clots, which can be seen under a microscope. "In normal blood clots, these fibres would look like a bowl of spaghetti" explained Pretorius. "But in diseased individuals, their blood clots look matted with large fused and condensed fibres. They can also be observed with special stains that fluoresce in the presence of amyloid."
The investigators have confirmed that this aberrant clot structure can be observed in all inflammatory diseases they have assessed, which now includes type 2 diabetes. However, the connection between bacteria, LPS, TLA and abnormal clotting, is unknown.
A recent study by Pretorius and Kell with University of Pretoria student Sthembile Mbotwe looked at an associated molecule, LPS-binding protein (LBP), found normally in everyone. LPS causes abnormal clot formation when added to the blood of healthy people, or the blood of patients with T2D. LBP can reverse that effect, as confirmed by microscopy. That has led the researchers to conclude that bacterial LPS is a major influence in the development of T2D.
"In an inflamed situation, large amounts of LPS probably prevent LBP from doing its work properly," explains Pretorius.
This work could have interesting implications for the treatment of these diseases. "We now have a considerable amount of evidence, much of it new, that in contrast to the current strategies for attacking T2D, the recognition that it involves dormant microbes, chronic inflammatory processes and coagulopathies, offer new opportunities for treatment," the researchers concluded.
Sources: Science Daily via Stellenbosch University, Scientific Reports