West Nile Virus May Now Have a Treatment
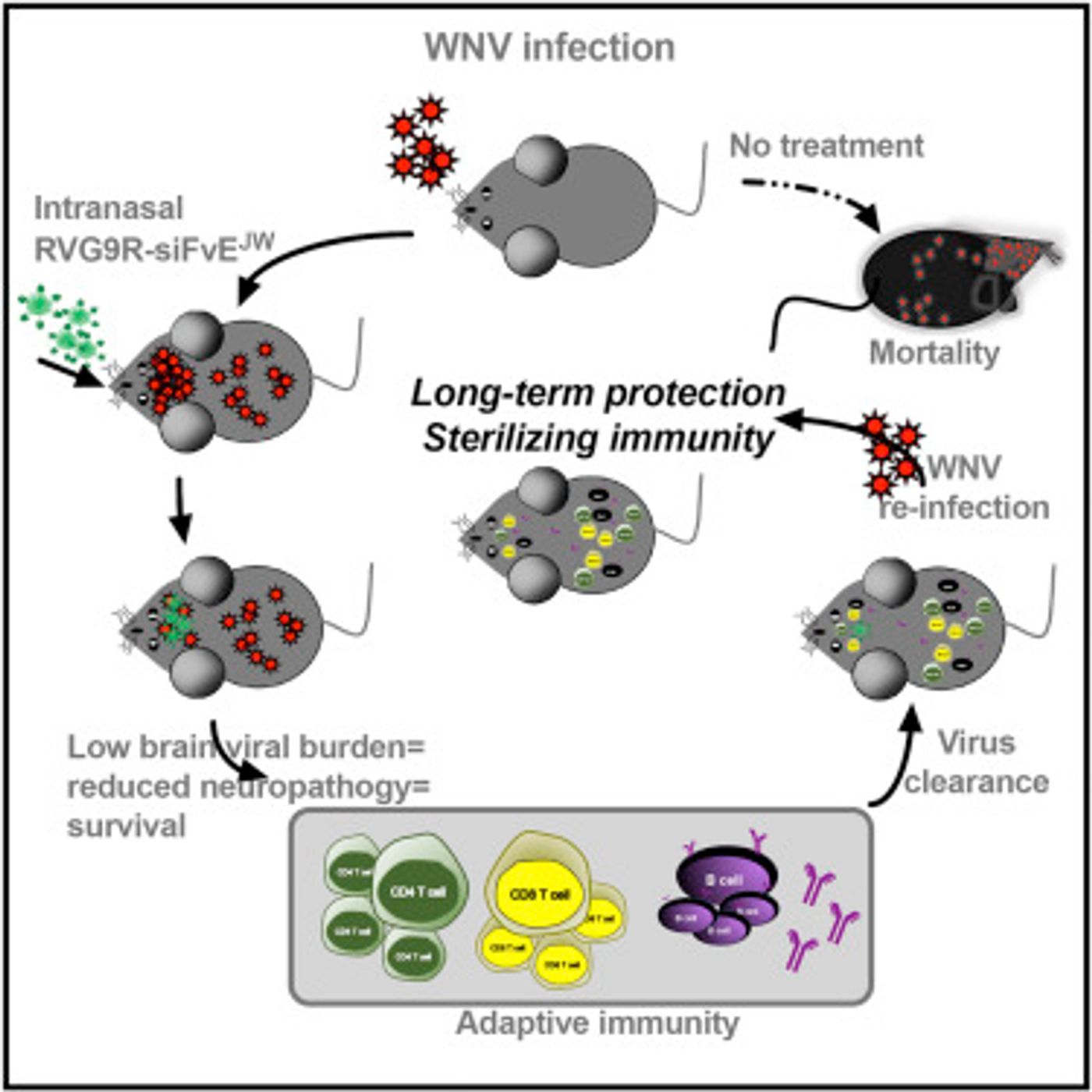
West Nile Virus is a mosquito-borne disease with no effective treatments and no vaccine. Often, there are no symptoms, but about one in five infected people gets a fever, and in about one of every 150 infected individuals, a severe and sometimes deadly disease develops. Now, scientists at Yale have created a therapy for the disorder; RNA molecules that were delivered through the nose have successfully treated mice that were infected with the virus.
Reporting in Cell Host & Microbe, the investigators found that the RNA therapy lowered the viral levels in the brains of the affected. That gave the immune system an opening, so it was able to kill the virus while also developing protection against it, shield from the pathogen in the long-term, the scientists said.
This research may be a strategic breakthrough for patients. While some don't even know they are infected, in others, West Nile Virus can cause serious damage once it has invaded the brain and the central nervous system. That wild variation in presentation has made therapeutic development very challenging, said senior author Priti Kumar, M.D., an associate professor of infectious disease at Yale School of Medicine.
When viruses infect cells, they take over the machinery inside and use it to make proteins for their own purposes.
The team focused on a molecule that had already been synthesized in the Kumar lab to try to find a West Nile Virus treatment; it was a small interfering RNA molecule, which can disrupt RNA translation (when messages are sent from the genome so that proteins can be made). In this work, the RNA works against several flaviviruses from mosquitoes. The scientists had to package the RNA, and in this case, used a peptide made from a virus so it would be able to enter neurons. Next, it had to be made for delivery through the nose.
When tested on mice, the new treatment worked well. It prevented harm to brain cells by reducing virus levels in the brain. The mice also had a 90 percent survival rate when compared to mice that only received a placebo. The immune system also developed a memory of the infection, shielding against future exposure.
The treatment "prevents pathology in the brain and gives the mice a chance to develop a robust immune response," said Kumar.
The researchers are hopeful this will lead to a therapy for humans. "In translation, it should be an effective strategy for people," she said.
If this works, the method could be used for treating other mosquito-borne illnesses, like St. Louis encephalitis, Japanese encephalitis, and maybe Zika, concluded the researchers.
Sources: AAAS/Eurekalert! Via Yale University, CDC, Cell Host & Microbe