Understanding how the Microbiome is Built
In our gastrointestinal tract, there are millions of microbes that help us digest food and get the nutrition we need. This community of microorganisms has a major influence on our health and well-being, and has been linked to the development and prevention of disease. But our immune system is designed to protect us from bacterial infection, so how is this microbial community, called the microbiome, established in the first place? Researchers at Caltech sought to answer that question. Reporting in Science, the team has found that one particular kind of bacterium acts to control the immune system, allowing microbes to settle into the gut, undisturbed.
In the lab of Sarkis Mazmanian, the Luis B. and Nelly Soux Professor of Microbiology and Heritage Medical Research Institute Investigator, graduate student Gregory Donaldson studied the microbe Bacteroides fragilis, which has been connected to human disease. There are multiple strains of this bacterium. Healthy people have been found to carry only one strain over the long-term. In addition, previous work in the Mazmanian lab showed that this bacterium, commonly found in the large intestines, can protect mice from disorders like multiple sclerosis and inflammatory bowel disease.
"Studies by other labs have shown that most people carry the same strain of B. fragilis throughout their lives," noted Donaldson. "We wanted to understand at a molecular level how these bacteria are able to colonize the gut in a stable, long-term way."
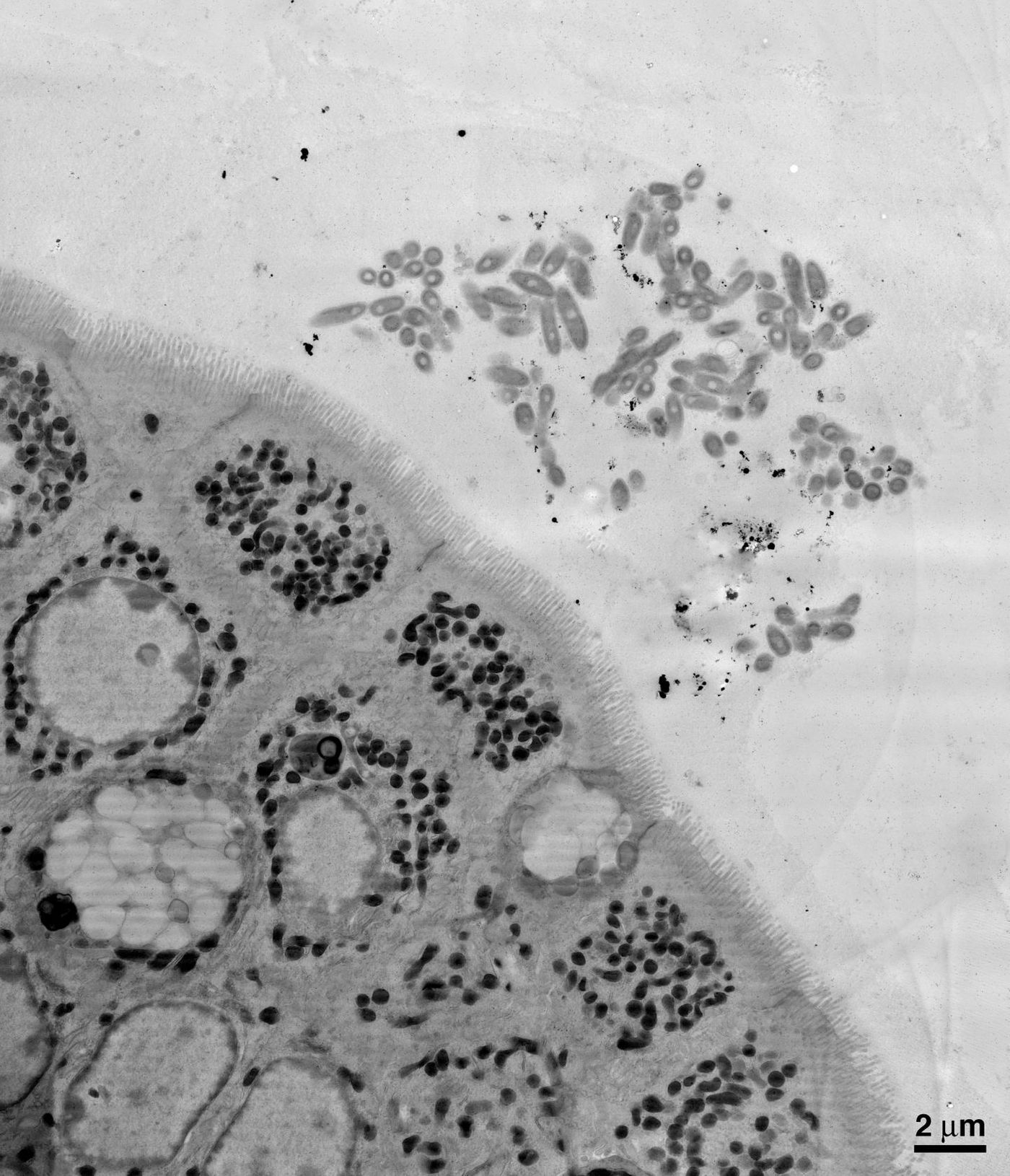
Using electron microscopy to find the bacteria, the investigators saw it clumping up in the layer of mucus that lines the gut, near cells that reside on the surface of the intestine. Each bacterium, they found, is encased within a carbohydrate capsule. Usually that capsule helps cloak dangerous bacteria, allowing it to evade the immune system. Without it, bacteria can’t take up residence in the mucus. Thus the researchers hypothesized that the capsule was necessary for B. fragilis to colonize the gut and establish themselves as the dominant strain.
The investigators determined, however, that a kind of immune protein that recognizes invaders and marks them for destruction, immunoglobulin A or IgA, would react to these capsules. IgA is everywhere in the gut, but its role is poorly understood. When it comes to B. fragilis, however, IgA was observed to actually assist the bacterium, helping it stick to the cells lining the intestine.
When they looked at the guts of mice that had no IgA, indeed, the bacterium had a tough time establishing itself in the gut.
"It is surprising to find that an immune response actually helps beneficial bacteria to thrive, which in turn helps the host thrive," said Donaldson. "The study of immunology has mainly been in the context of pathogenic bacteria. But there are trillions of bacteria in the gut, and most of the time none of them are making you sick. Our study shows that there is active immune recognition of these bacteria, but it helps rather than hinders them. This suggests that the immune system is more than just a defense system and antibodies are more than just weapons."
In the video above, Sarkis Mazmanian discusses how the microbiome might be used to relieve disease.
The scientists plan to continue this work; they want to learn more about why B. Fragilis is tolerated while other bacteria are attacked. The aim is to help beneficial bacteria grow in the intestines, which might help treat some diseases.
"Over the past decade, many studies have profiled the gut microbiome in a variety of diseases, lifestyles, geographies, and following birth," said Mazmanian. "We've learned that the community composition of the microbiome correlates with particular conditions--for example, altered microbiome configurations may contribute to inflammatory bowel disease, autism, and Parkinson's disease. What has remained largely unknown is how a microbiome is established and maintained in the first place. Our study reveals a molecular mechanism by which specific beneficial bacteria actively promote long-term intestinal colonization by engaging and co-opting the immune system, rather than trying to evade it as pathogens do. This discovery may lead to new ways to correct microbiome imbalances, and perhaps to prevent and treat a variety of human disorders."
Sources: AAAS/Eurekalert! Via Caltech, Science