Rise of Antibiotic Resistance Linked to Climate Change
There are several factors blamed for the rise of antibiotic resistance, which already causes the deaths of around 23,000 Americans a year and is considering to be a rising threat to public health. Antibiotics are prescribed too commonly, and people don’t have good habits when it comes to taking them as directed, two major reasons why drugs now don’t work as well when it comes to fighting common pathogens. But new research suggests that environmental pressures may be playing a role. An international team of researchers from a variety of fields has found that population density and higher temperatures are linked to an increase in numbers of bacteria carrying antibiotic resistance genes. Their work has been reported in Nature Climate Change.
"The effects of climate are increasingly being recognized in a variety of infectious diseases, but so far as we know this is the first time it has been implicated in the distribution of antibiotic resistance over geographies," said the lead author, Derek MacFadden, MD, an infectious disease specialist and research fellow at Boston Children's Hospital. "We also found a signal that the associations between antibiotic resistance and temperature could be increasing over time."
"Estimates outside of our study have already told us that there will already be a drastic and deadly rise in antibiotic resistance in coming years," said the co-senior author John Brownstein, PhD, who is Chief Innovation Officer and director of the Computational Epidemiology Group at Boston Children's and professor of pediatrics at Harvard Medical School (HMS). "But with our findings that climate change could be compounding and accelerating an increase in antibiotic resistance, the future prospects could be significantly worse than previously thought."
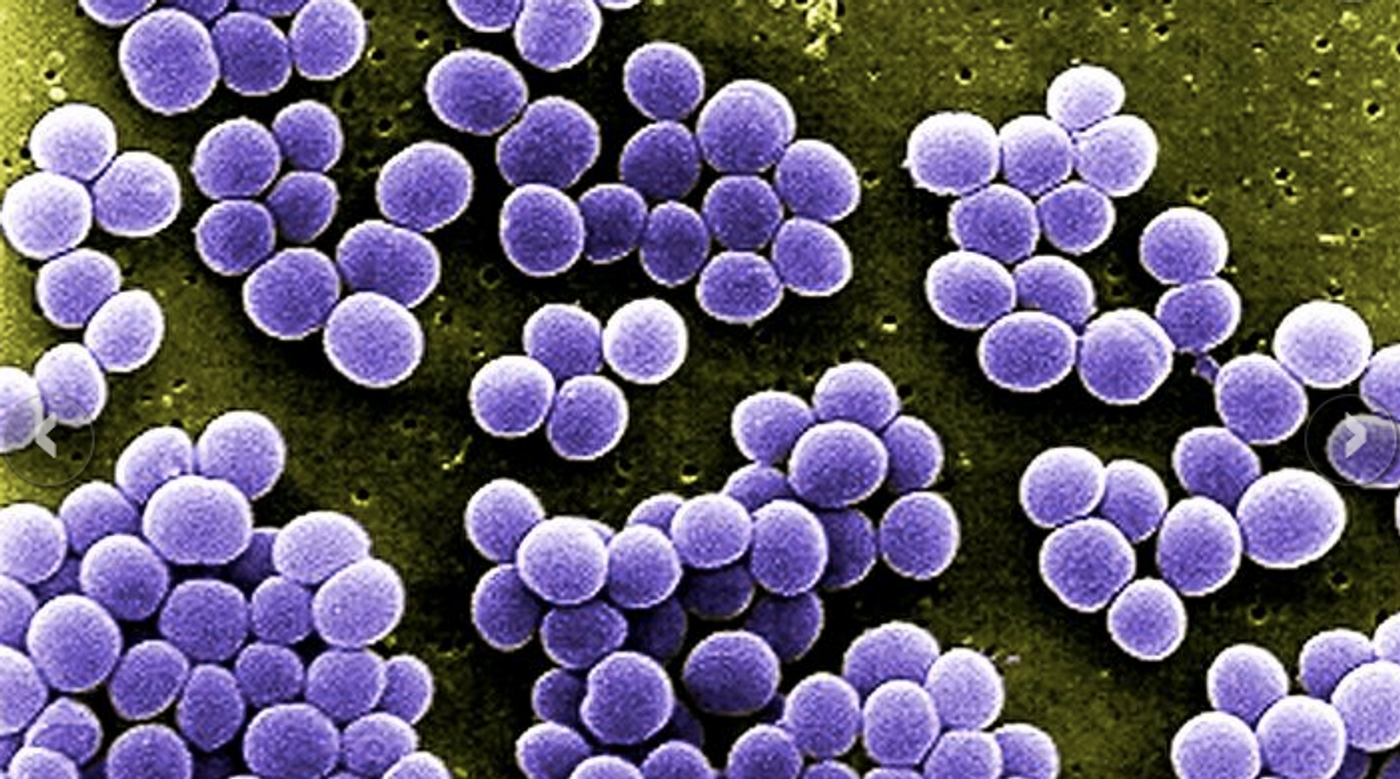
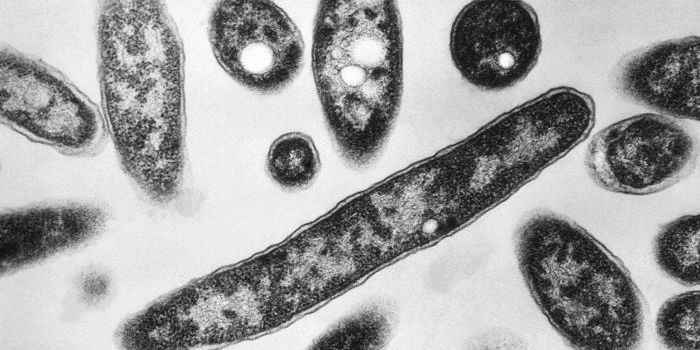
The researchers developed a database about the incidence of resistance in several strains of bacteria in the United States, including K. pneumoniae, S. aureus, and E. coli. Data was collected from labs, researchers, and hospitals, ultimately containing 1.6 million bacterial pathogens from 602 records made between 2013 and 2015, across 223 facilities and 41 states.
The investigators confirmed that an increase in the rate of antibiotics prescribed is linked to an increase in antibiotic resistance, for every microbe they assessed.
The team found a strong correlation between antibiotic resistance and average minimum temperatures as well. A ten Celsius degree increase in minimum temperature was connected to increases in resistance; for a strain of E.coli (a 4.2% increase), K. pneumoniae (2.2%), and S. aureus (3.6%).
Additionally, an increase in 10,000 people within a square mile increased resistance by three and six percent, respectively, in E. coli and K. pneumoniae. S. Aureus did not appear to be impacted by population density.
"Population growth and increases in temperature and antibiotic resistance are three phenomena that we know are currently happening on our planet," said the study's co-senior author Mauricio Santillana, Ph.D., who is a faculty member in the Computational Health Informatics Program at Boston Children's and an assistant professor at HMS. "But until now, hypotheses about how these phenomena relate to each other have been sparse. We need to continue bringing multidisciplinary teams together to study antibiotic resistance in comparison to the backdrop of population and environmental changes."
"As transmission of antibiotic-resistant organisms increases from one host to another, so does the opportunity for ongoing evolutionary selection of resistance due to antibiotic use," MacFadden added. "We hypothesize that temperature and population density could act to facilitate transmission and thus increases in antibiotic resistance."
"The bottom line is that our findings highlight a dire need to invest more research efforts into improving our understanding of the interconnectedness of infectious disease, medicine, and our changing environment," Brownstein concluded.
The video above is a Ted talk about the threat of antibiotic resistance.
Sources: AAAS/Eurekalert! Via Boston Children’s Hospital, Nature Climate Change