Rupture of small blood vessels in the brain can cause hemorrhagic stroke and brain microbleeds, and finding the fastest repair mechanisms is the best way to treat these conditions. In a new study from Southwest University in China, researchers have discovered for the first time the unique role of macrophages in the repair broken blood vessels.
Vessels have the potential to rupture all over the body, but when they break in the brain, the damage is directly associated with cognitive decline from neurodegenerative diseases. Brain bleeds, detectable by MRI, are most common in elderly people, especially with dementia or cerebrovascular disease, but they can happen to anyone. Until the current study, published in
Immunity, scientists were unsure about the level of capability the brain had to repair broken vessels.
The research team from China used a multi-photon laser in a large zebrafish study to visualize how the organisms responded to vascular injury. The laser cleanly ruptured small blood vessels in the zebrafish brains, creating two clearly broken ends. Using a specialized microscope, the scientists incorporated in vivo time-lapse imaging to see how the vessels were repaired.
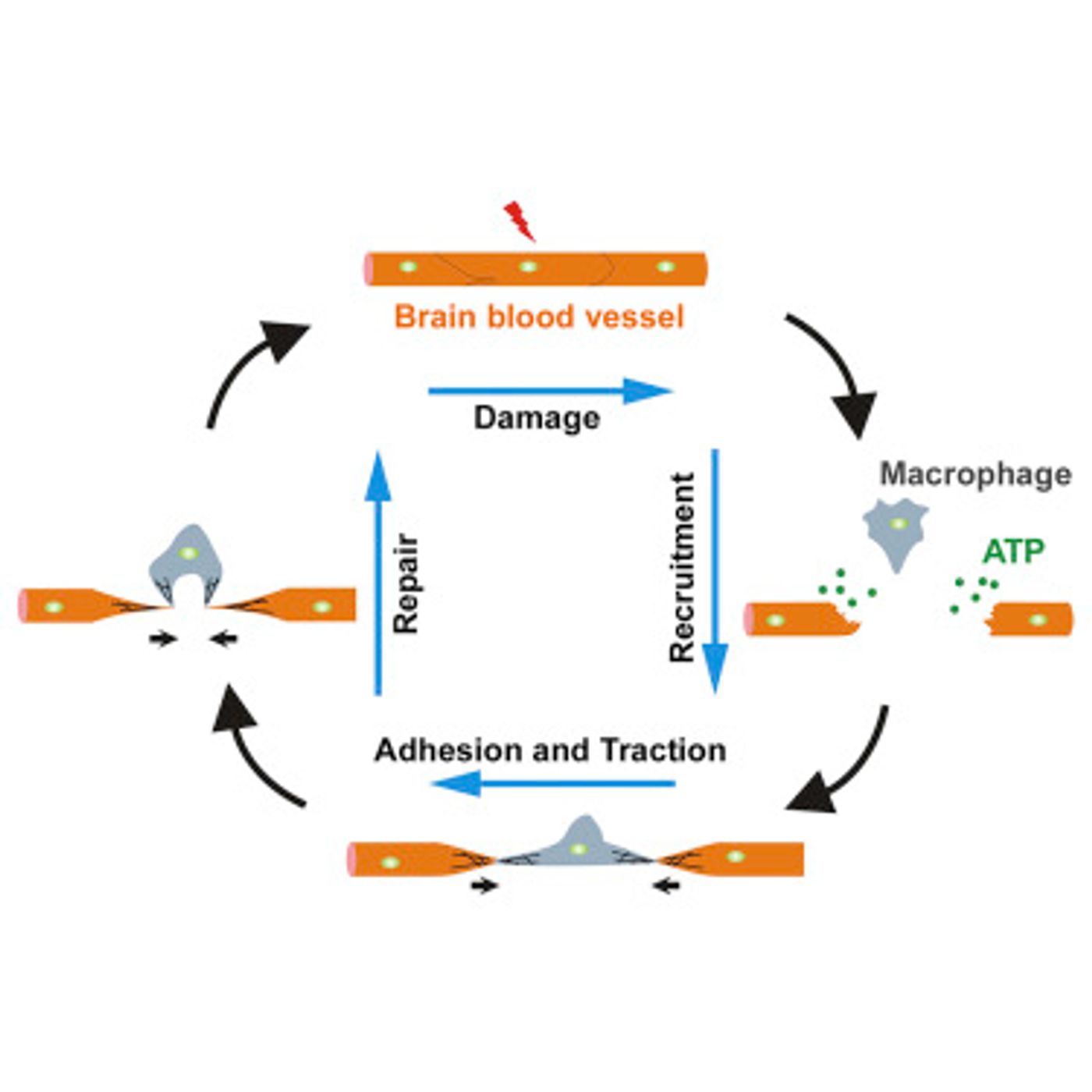
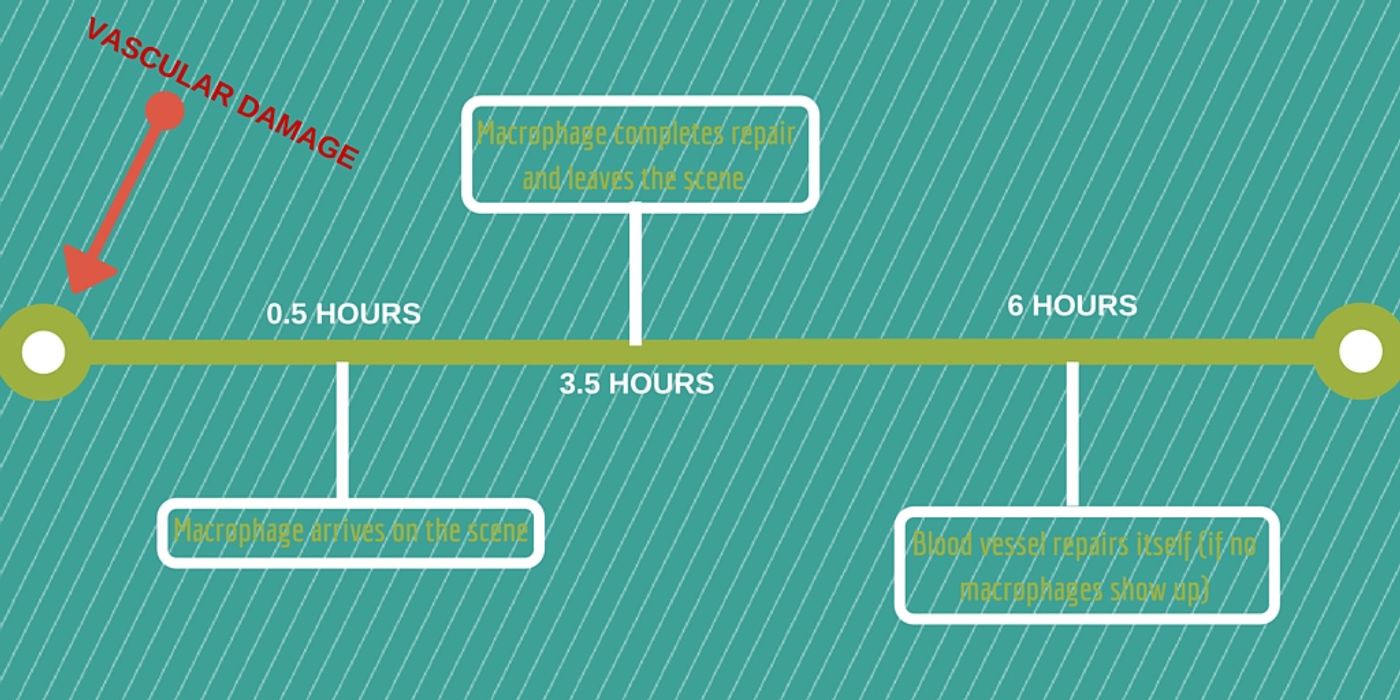
Approximately 30 minutes post-laser injury, a white blood cell called a macrophage arrived to the scene of rupture. These cells of the immune system are present in virtually every tissue of the body, providing multiple services relating to cellular clean-up, production of immune effector molecules, and engulfing harmful pathogens.
Upon arrival, the macrophage used two arm-like extensions, called filopodia or lamellipodia, to connect to both of the broken ends of the blood vessel. During a period of three hours, the macrophage reattached the broken ends using secreted adhesion molecules from the damaged blood vessel.
“We confirmed that the macrophage mediates this repair through direct physical adhesion and generation of mechanical traction forces,” said PhD student Chi Liu. “This is a previously unexpected role of macrophages."
In addition to the macrophage repair seen in the zebrafish brain, similar repair occurred in ruptured blood vessels in the zebrafish fin. Another rare occurrence is two macrophages responding to the distress call emitted by ruptured small blood vessels. In this case, both of the macrophages begin the process but then quit, as if they left because they thought the other macrophage had the job covered. Additionally, there is a chance of microfilament depolymerization and inhibition of phosphatidylinositide 3-kinase (PI3K) or Rac1 activity. Researchers saw that these events disrupted macrophage-endothelial adhesion.
Lastly, the researchers also saw that zebrafish blood vessels can repair themselves independently of macrophages, but the process is much slower and less efficient.
Other aspects of vascular development and remodeling are shared between zebrafish and humans, so scientists are hopeful that this discovery will also be seen in humans. Further studies backing up this hypothesis will soon help scientists improve treatments for human vascular repair.
Sources:
Lancet Neurology, Nature Reviews Immunology, Immunity, Cell Press/Southwest University