A New Understanding of How Scars Form
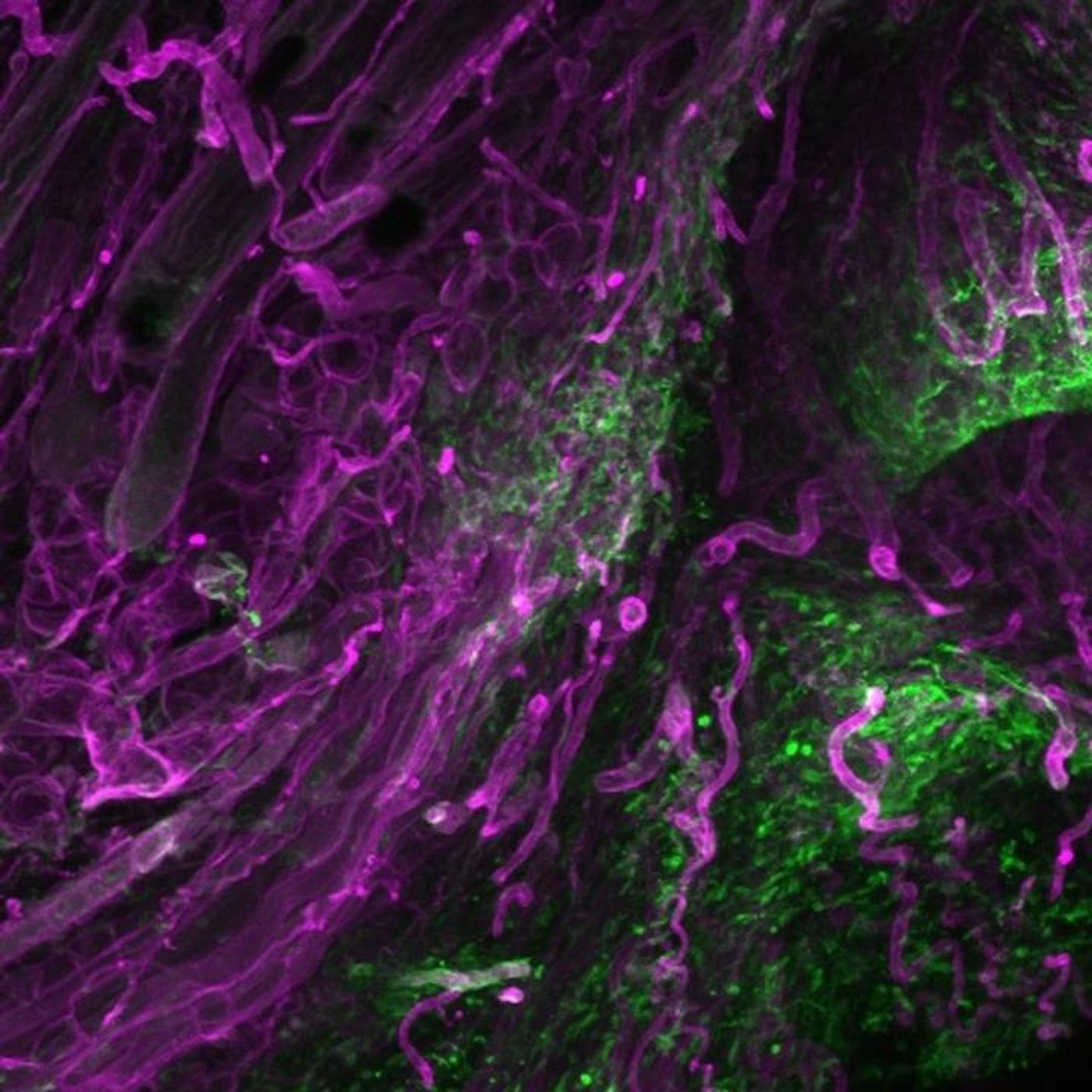
It was thought that when skin is wounded and a scar is formed, a cell called a fibroblast, which is a kind of connective tissue, moves to the site of the wound and leave plugs to generate a three-dimensional structure called an extracellular matrix. Chronic wounds that don't heal or fibrosis involve abnormal scarring, which can be a serious threat to health. Scientists have sought to learn more about where these fibroblasts come from and the exact role they play in scarring.
Researchers knew that scar formation involves a specific type of fibroblast that expresses a gene called Engrailed-1. This lineage of cells is present in skin as well as fascia, a sheet of connective tissue that sits below the skin. Scientists led by Dr. Yuval Rinkevich, Group Leader for Regenerative Biology at the Institute of Lung Biology and Disease at Helmholtz Zentrum München wanted to know more about how the scarring process was controlled. They used a variety of molecular techniques including genetic ablation.
In their work, the researchers were able to eliminate the fascia fibroblasts. When they did so, wounds did not incorporate an extracellular matrix, and only unhealthy scars that were dysfunctional were able to form. The investigators also prevented fascia fibroblasts from moving to the skin by applying a porous film under the skin, which caused chronic open wounds.
Their experiments led the research team to conclude that within fascia is a set of fibroblasts that sits inside a sealant that can migrate; this assembles various necessary biological tools, including different cell types and a matrix that the body uses to heal wounds. The work has been reported in Nature.
"The findings of our research give fascia tissue a new role for future science. This will shift the attention of the scientific community to not only to look at fibroblasts in the dermis but also at native cells in the fascia when researching on wound healing," said Rinkevich.
This study has indicated that when scars form in mammals, the injury causes a universal response that uses fibrotic tissue to heal wounds rapidly with scars. This stops infections and prevents excessive bleeding. It had been thought that scars are caused when fibroblasts leave an extracellular matrix at the site of a wound. In actuality, scars seem to form when sentry fibroblasts that reside in the fascia move a reservoir of matrix jelly to open wounds.
The mechanism that the researchers have revealed may help scientists prevent pathological fibrosis, and initiate scarless healing.
"Our new findings challenge and reconfigure the traditional view of the body's matrix system of connective tissue. This is opening up a new biological concept that radiates to a variety of aspects of scar-related disease," said the co-first author of the report Donovan Correa-Gallegos, a graduate student at Helmholtz Zentrum München.
Learn more about chronic wounds from the video.
Sources: AAAS/Eurekalert! via Helmholtz Zentrum München - German Research Center for Environmental Health, Nature