Potential Treatment for Brain and Spinal Cord Injury is IDed
There are a limited number of treatment options for people that have suffered swelling-inducing injuries to their brain and spinal cord. The condition, called central nervous system (CNS) edema, can only be treated now with a medically induced coma or high-risk surgery. Injuries and trauma that cause this disorder can affect people of all ages, though older people tend to fall more often than younger people and, therefore, suffer more CNS edema. Young people that are impacted often have years of recovery ahead of them.
A new treatment could change the prognosis for the estimated 75 million patients that are affected by CNS edema every year. Reported in Cell by an international team of researchers, an approved anti-psychotic medication called trifluoperazine (TFP) was shown to change tiny water channels in cells called aquaporins, which has a therapeutic effect in a CNS edema model.
When there is a sudden loss of oxygen to the CNS, ions build up in cells, causing water to rush through aquaporins and into cells to reduce this 'saltiness,' swelling the cells. The swollen cells start exerting pressure on the spine and skull, damaging tissue and disrupting the electrical signals that move between the brain and the body.
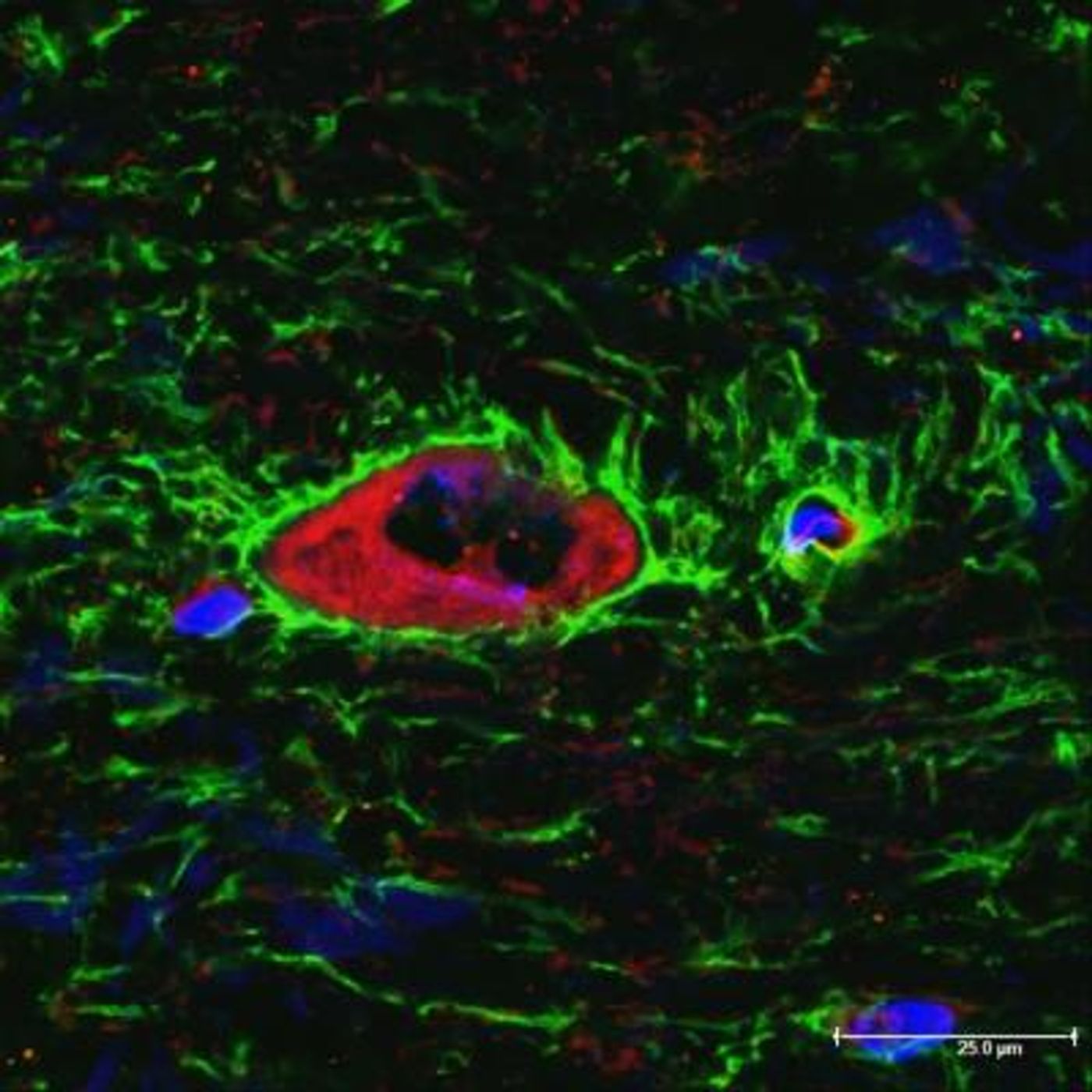
TFP can stop this process. In a type of brain cell called astrocytes, a protein called calmodulin normally attaches to the aquaporins and sends them to the cell surface, allowing more water in. But TFP stops calmodulin from binding aquaporins, which stops them from moving to the cell surface, preventing the cells from swelling with water. The drug was tested in rats, and a single dose enabled them to recover from an injury in two weeks, while injured but untreated rats spent more than six weeks recovering.
More work will be needed to confirm these findings in people, but it could be a huge benefit to CNS edema patients, especially since the drug has already been approved for a different use. The short-term nature of this treatment - only one dose may be needed for a benefit - also reduces the potential side effects dramatically.
"Every year, millions of people of all ages suffer brain and spinal injuries, whether from falls, accidents, road traffic collisions, sports injuries, or stroke. To date, their treatment options have been very limited and, in many cases, very risky," said Professor Roslyn Bill of the Biosciences Research Group at Aston University.
"This discovery, based on a new understanding of how our cells work at the molecular level, gives injury victims and their doctors hope. By using a drug already licensed for human use, we have shown how it is possible to stop the swelling and pressure build-up in the CNS that is responsible for long-term harm," Bill added. "While further research will help us to refine our understanding, the exciting thing is that doctors could soon have an effective, non-invasive way of helping brain and spinal cord injury patients at their disposal."
"This is a significant advance from current therapies, which only treat the symptoms of brain and spinal injuries but do nothing to prevent the neurological deficits that usually occur as a result of swelling. The re-purposed drug offers a real solution to these patients and can be fast-tracked to the clinic," said Dr. Zubair Ahmed of the University of Birmingham's Institute of Inflammation and Ageing.
"This novel treatment offers new hope for patients with CNS injuries and has huge therapeutic potential. Our findings suggest it could be ready for clinical application at a low cost in the very near future," added Dr. Mootaz Salman, Research Fellow in Cell Biology at Harvard Medical School.
Sources: AAAS/Eurekalert! via Aston University, Cell