One major benefit of stem cells is that they could be used to create healthy cells of any type. In the lab, skin cells have already been converted into liver cells, kidney cells and heart cells among other cell types. One day it may be possible to replace organ transplantation with such cells. A serious challenge remains, however, in successfully getting those cells inside a patient with a failing organ.
Researchers at University of California San Francisco (UCSF) have now
reported that in mice, they have simply changed diseased liver cells inside an animal. That means bypassing the process of grafting new cells as well as the added benefit of reducing unhealthy cells by converting them into healthy cells, thereby improving liver function.
The method they used took advantage of a delivery system that is already approved for use in humans, so it’s possible that this new technique could quickly be translated into a treatment for people afflicted with liver disease.
“Part of why this works is that the liver is a naturally regenerative organ, so it can deal with new cells very well. What we see is that the converted cells are not only functionally integrated in the liver tissue, but also divide and expand, leading to patches of new liver tissue,” said Holger Willenbring, associate director of the Liver Center at UCSF and an author of this new
study, which was published in the journal Cell Stem Cell.
According to the National Institute of Diabetes and Digestive and Kidney Diseases, people often have no symptoms of liver disease until it progresses to irreversible scarring, called cirrhosis. At that point, treatment options are fairly limited and efforts mainly are aimed at preventing the disease from deteriorating into liver failure. Over 600,000 people in the United States have end-stage liver disease. With the only cure being liver transplantation, only about 6,000 people are able to use that option, leaving more than 35,000 people to die of the illness and making it the 12th leading cause of death by disease in the U.S. Since obesity is a cause of cirrhosis, that number is likely to increase.
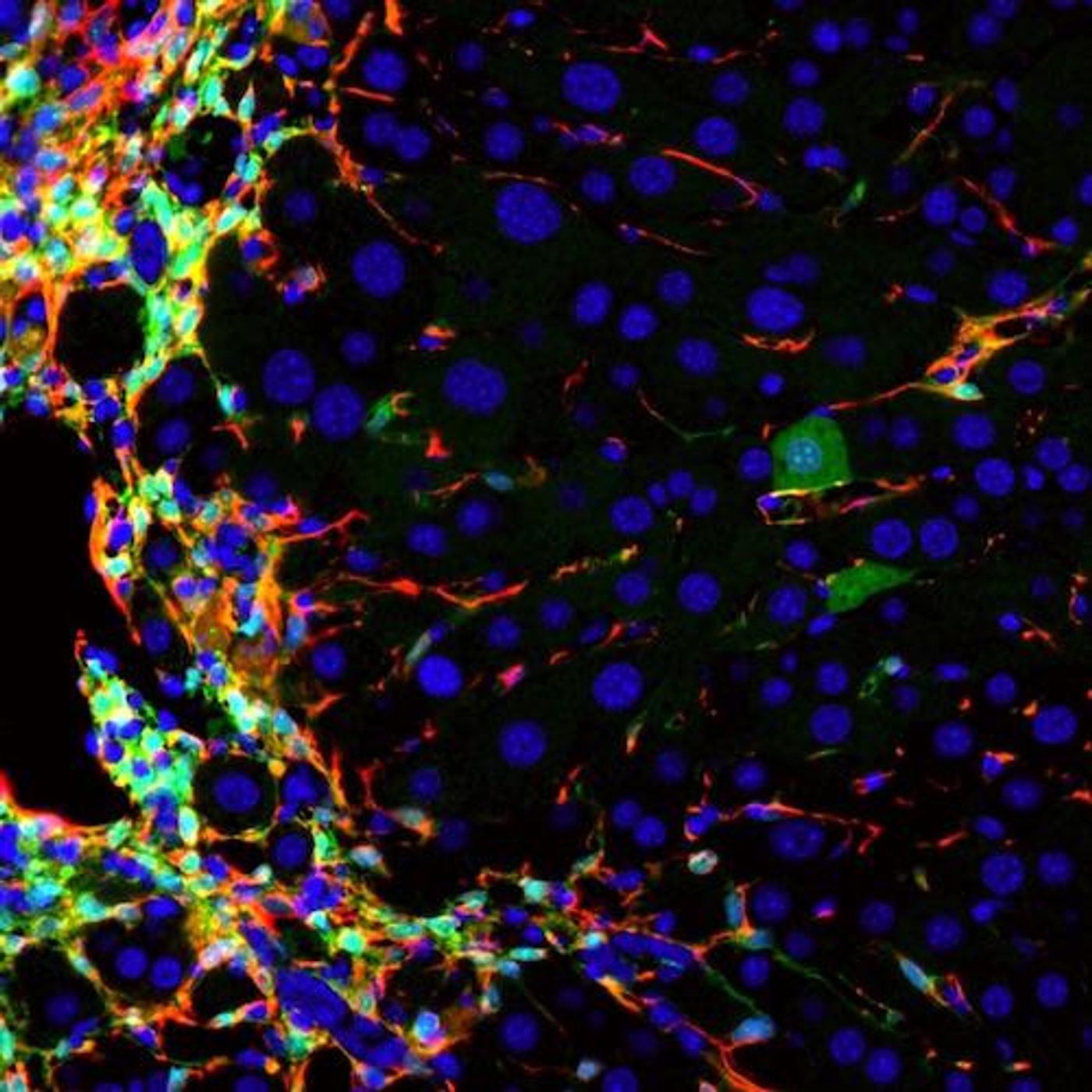
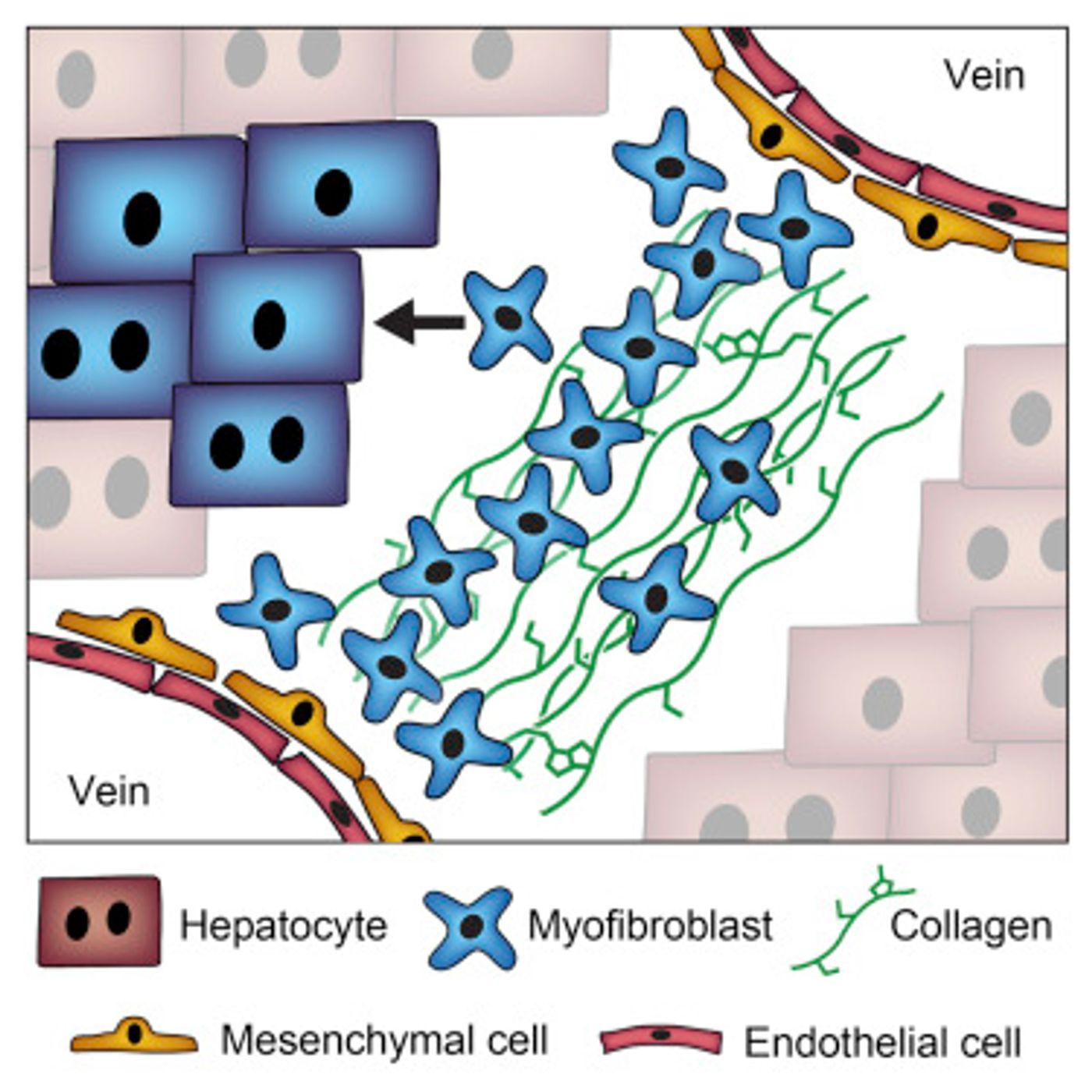
The new treatment technique targets the scarring of the liver that drives liver disease. When liver cells, called hepatocytes, can't repair the damage done by toxins like alcohol or diseases such as hepatitis C, they die off and cannot regenerate. Gaps are then left by the dead cells that are filled with scar-like fibrotic tissue. At first these little bandaids are good for maintaining the structural integrity of the liver, eventually they are too numerous compared to the number of hepatocytes, inhibiting the normal activity of the organ and causing it to fail.
While Willenbring has worked for years on how to use stem cells in place of transplants, there has been a realization that the tangle of scar tissue in the liver inhibits successful growth of transplanted cells, and this approach could fail. His team, along with collaborators, has identified a cocktail of proteins that cause cells to convert into hepatocytes. Once they found a way to infect scar tissue in the liver with the cocktail, they demonstrated the conversion of that tissue into hepatocytes in cells of a mouse liver. That number of converted cells was very small, only about one percent, but that was enough to improve liver function.
More work is needed to refine and improve the methodology and results; it has the potential to be an efficient therapy, and commonly available at low cost. Willenbring acknowledges that the current standard of care in liver disease should not yet be supplanted. “A liver transplant is still the best cure,” Willenbring explained. “This is more of a patch. But if it can boost liver function by just a couple percent, that can hopefully keep patients’ liver function over that critical threshold, and that could translate to decades more of life.”
Learn more about cirrhosis in the video below.
Sources:
NIDDK,
UCSF via
AAAS,
Cell Stem Cell