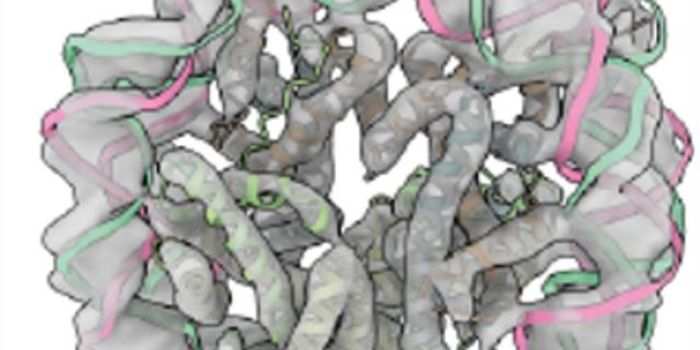
A team at Dana Farber/Boston Children’s has been able to selectively silence a gene, BCL11A, found in 2008 to be an integral part of a potential Sickle Cell cure using gene therapy.
Sickle Cell Disease affects about 300,000 babies worldwide every year. The disease is a result of a gene mutation in hemoglobin, an oxygen-carrying molecule in red blood cells. Hemoglobin is well-known for giving blood its red color due to the iron it contains.
The mutation,
discovered in 1956 by Vernon Ingram and colleagues at the University of Cambridge, causes red blood cells to have a crescent shape. This altered shape gives them less ability to carry oxygen and results in cell clumping. Patients can suffer from anemia, organ failure, stroke, infection, and severe pain.
Since the mutation and “cause” of the disease had been discovered, scientists thought they were on an easy road to treatment. However, this has not been the case. Few labs study the disease and funding is not as easy to come by as other more ‘high profile’ diseases.
There is only one FDA-approved drug to treat the disease. Hydroxyurea is an old cancer drug that was found by chance to quell the extremely painful episodes observed in patients, called sickle cell crisis, but only works in about half of sickle cell patients and has very serious side effects. The other route patients can take is to have a full bone marrow transplant to cure the disease. Even if patients are able to find a match, the procedure has a 5% fatality rate and requires an ongoing regimen of anti-rejection drugs.
Crossing the “Valley of Death”
The issue has been the gap between knowing the mechanisms of the disease and figuring out a treatment, known by researchers as the “valley of death” for the long amounts of time taken and uncertainty in finding a cure.
Around the time that the mutation was first discovered, scientists realized that the reason some patients have very few if any symptoms and others are debilitated by the disease, is due to fetal vs adult hemoglobin types. Those patients still able to produce fetal hemoglobin, which usually is switched to the adult version early in life, have fewer symptoms than those who only make adult hemoglobin. It is this fetal hemoglobin that keeps the disease at bay.
The test has been to work out how to suppress adult hemoglobin production and increase fetal hemoglobin levels in patients without serious immune side effects.
Gene therapy to the rescue! Even though gene therapy is still in a trial stage in most cases, it holds promise for treatments and cures in a variety of diseases. Thanks to the tenacity of Dr. Stuart Orkin and colleagues at Dana Farber/Boston Children’s, the long awaited potential for a cure is finally here.
Dr. Orkin has been working on blood cell development and blood disorders for decades. In 2008, a student in Dr. Orkin’s lab, Vijay Sankaran, finally found the gene responsible for turning on adult hemoglobin, BCL11A. By suppressing this gene, cells turned to making an increased amount of fetal hemoglobin and sickle cell disease disappeared in cell culture and in mice.
Trial for a Cure
Now, a team led by
Dana-Farber/Boston Children’s researchers David A. Williams, MD, Christian Brendel, PhD, and Swaroopa Guda, PhD, engineered a virus that suppresses BCL11A selectively, only in red blood cell precursors. They found it was important to work with BCL11A in blood stem cells and not all red blood cells because the total suppression of the gene would affect long term stability of blood development in general. By using gene therapy to target only blood stem cells, BCL11A is silenced resulting in reduced signs of the disease.
“BCL11A represses fetal hemoglobin, which does not lead to sickling, and also activates beta hemoglobin, which is affected by the sickle-cell mutation. So when you knock BCL11A down, you simultaneously increase fetal hemoglobin and repress sickling hemoglobin, which is why we think this is the best approach to gene therapy in sickle cell disease,” explained Williams, the study’s senior author and president of Dana-Farber/Boston Children’s.
Selectively suppressing BCL11A required complex genetic engineering. Researchers combined the core of the therapy, a short hairpin RNA (shRNA) that inactivates the BCL11A gene, with a microRNA that cells easily recognize and process, a beta hemoglobin promoter, and some red blood cell precursor regulatory elements to ensure processing within the right cell types. This hybrid construct was then inserted into a lentivirus, powerhouses for delivering genetic material to cells, proved safe for use in human patients. Once mixed with cells from sickle cell patients, the lentivirus delivered the therapy and cells began producing fetal hemoglobin as expected.
Not only does this provide a solid foundation for a successful clinical trial, it also opens up the doors to other successful therapies. Dr. Williams notes that this approach can be used in other blood disorders, such as beta-thalassemia. The team is working toward FDA approval for the trials to start in early 2017.
Sources:
Harvard Gazette,
StatNews,
Nature,
Dana Farber/Boston Children's