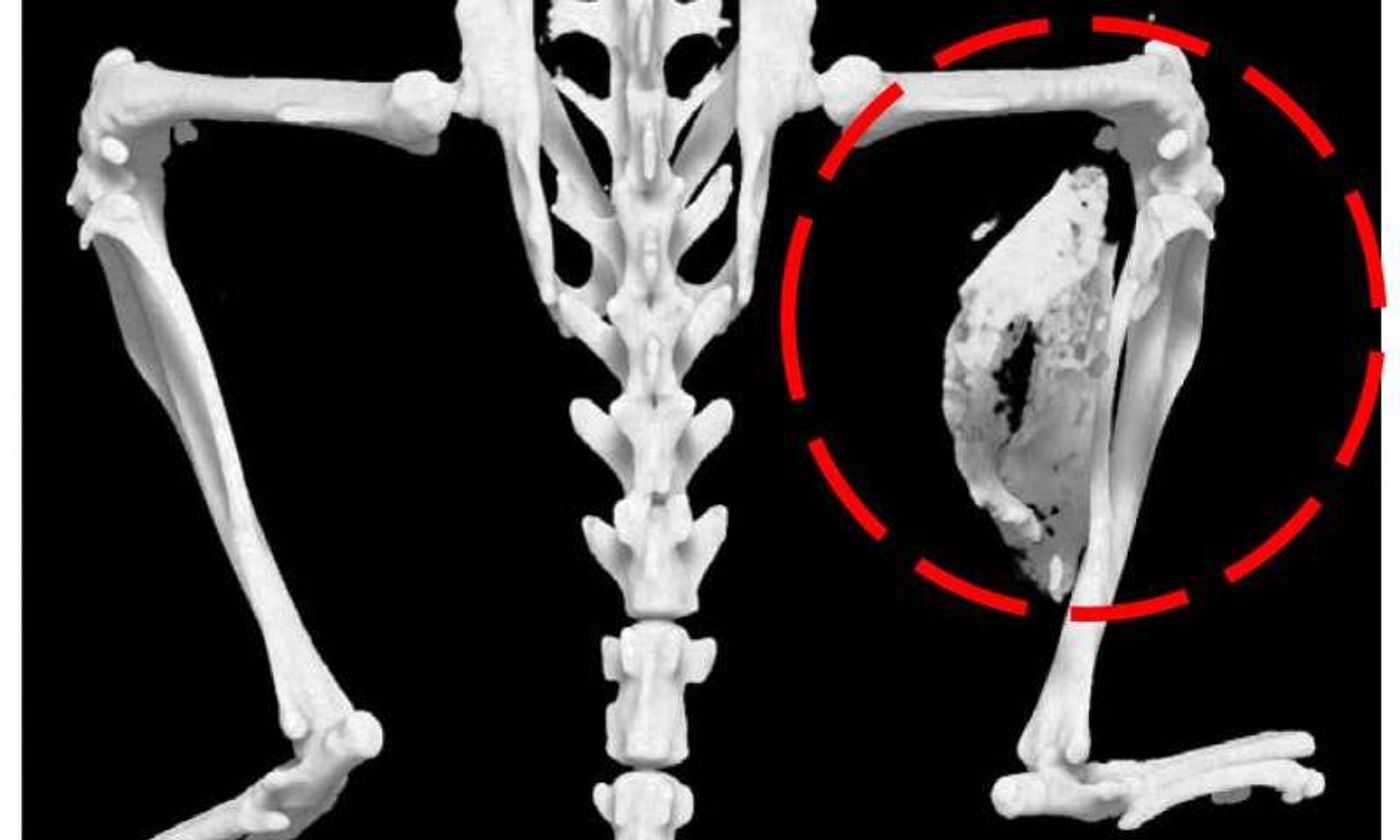
Fibrodysplasia ossificans progressiva (FOP) is an extremely rare genetic disease that causes bone to grow in abnormal areas like ligaments, tendons, and skeletal muscles. This atypical growth causes soft tissues to "undergo a metamorphosis" transforming normally flexible tissues into hard bone, "locking joints in place and making movement impossible" (
National Organization for Rare Disorders).
In the past, treatment for this debilitating disorder included targeting the signaling pathway of bone morphogenetic proteins (BMPs), since the hyperactivity of these multi-functional growth factors is the root cause of FOP (
NIH). However, in a new study published in
PNAS, scientists from the Center for iPS Cell Research and Application (CiRA) at Kyoto University utilized the ability of induced pluripotent stem cells (iPSCs) to reprogram diseased cells in FOP patients.
iPSCs are listed by the
NIH as "adult cells that have been genetically reprogrammed to an embryonic stem cell–like state," meaning they are essentially identical donor cells that can be induced to differentiate differently, making them useful by scientists to repair diseased tissues.
People with the genetic mutation for FOP develop symptoms of the disease after experiencing inflammation or trauma. The team from CiRA aimed to utilize the reprogrammable iPSCs in FOP mouse models to identify a certain inflammatory molecule triggering FOP development and potentially reverse its effect.
Studying alternative treatments to BMP signaling drug targets introduces an entirely new perspective on FOP treatment. CiRA scientists believed that the abnormality of BMP signaling causing FOP could be either unconditional BMP activation or atypically enhanced signaling strength when BMP is activated. Looking closer at the cause of FOP BMP signaling, they identified the role of Activin-A, a member of the transforming growth factor-beta superfamily, in the onset of FOP (
NIH).
“Using iPS cell technology, the scientists found that only cells harboring the FOP gene mutation would respond to Activin-A by significantly increasing their BMP signaling," a report from Kyoto University stated.
Since immune actions in response to trauma trigger FOP, the treatment and study of FOP has historically been very complicated, seeing as surgical treatments to remove excessive bone only stimulate more irregular bone growth. The discovery of Activin-A's connection to BMP signaling offers a new method for repressing diseased bone growth in FOP patients and lends new information to the realm of drug discovery and bone growth in general.
Watch the following video to learn more about the clinical application potential of iPSCs.
Source:
Kyoto University