Detecting and Diagnosing Rheumatoid Arthritis Before it Begins
Unique gene signatures and tiny changes in the immune system that occur in the earliest stages of rheumatoid arthritis, an autoimmune disease, could soon be used to apply new diagnostic methods and provide early therapeutic intervention. From the European League Against Rheumatism (EULAR), scientists present their newest findings on how to identify which at-risk individuals will ultimately develop rheumatoid arthritis.
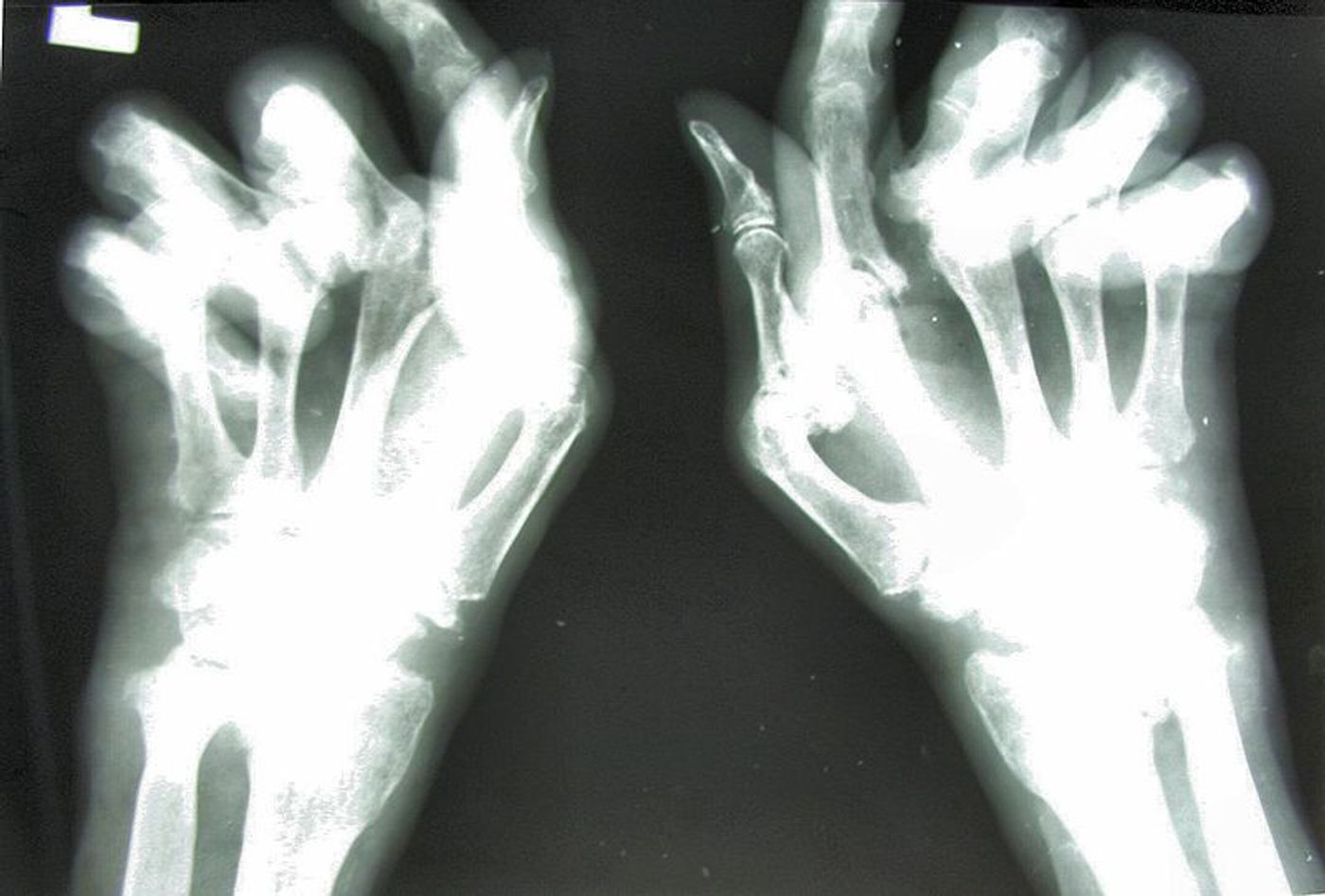
People with rheumatoid arthritis (RA) are plagued with chronic inflammation in the joints, often the hands, feet, wrists, elbows, knees, and ankles. Inflammation in the joints causes the synovium to thicken, the joint tissue responsible for lubricating the joints and allowing easy movement. This thickening is what leads to the swelling and pain experienced by RA patients. Findings from this study could one day lead to early therapeutic interventions that could prevent irreversible damage to the joints and inhibit progression of the disease.
When specific autoantibodies are discovered, a person is known to be an increased risk of developing RA, although the presence of these autoantibodies does not necessarily seal their fate. Autoantibodies are produced in many different autoimmune diseases. They represent a malfunction in the immune system, where B cells produce antibodies that target the body’s own cells and tissues instead of producing antibodies that target foreign invaders like bacteria and viruses.
"These studies may help us better understand and potentially identify which individuals classified as at-risk will go on to develop RA," explained EULAR’s Robert Landewé. "This is important because it will contribute to the development of early preventative strategies including potential pharmacological treatment to prevent the onset of disease."
Researchers began their study with 67 synovial tissue samples from the knee joint of individuals with an early risk of RA. With just 13 participants, they conducted a genome-wide transcriptional profile study aimed at identifying unique gene signatures associated with RA development. They found 3,151 gene signatures linked to elevated risk of RA and 2,437 signatures linked with a lower risk. They confirmed these results using a technique called quantitative real-time PCR.
"Our results clearly show molecular changes appearing in the synovial tissue before the onset of arthritis," said Dr. Lisa van Baarsen. "The characterization of these gene signatures will enable us to better understand the pathophysiology of the pre-clinical phase of the disease and potentially identify novel drug targets for preventive intervention."
In addition to classifying genetic risk biomarkers, researchers also observed changes in immune-regulated pathways involving T cells and B cells, cytokines and chemokines, and antigen processing and presentation.
"Our data support a new biomarker that demonstrates better predictive power compared with other available biomarkers evaluated so far," said Ms. Anne Musters, MD.
The findings from this study were recently presented at the Annual European Congress of Rheumatology.
Sources: Arthritis Foundation, European League Against Rheumatism (EULAR)