The key ingredient in the recipe that make staphylococcus and streptococcus infections so dangerous? Superantigen toxins. A new study from The Hebrew University of Jerusalem, twenty years in the making, showed how treatments for these infections could target the toxins instead of the bacteria themselves.
Study researcher Professor Raymond Kaempfer explained their approach to providing an alternative to targeting antibiotic-resistant bacterial infections:
"Rather than targeting the bacterial pathogens, which can then mutate to develop antibiotic resistance, host-oriented therapeutics have the advantage of remaining effective even against infections with antibiotic-resistant strains. This is because before the pathogens can cause severe disease, they must also pass through the same receptor bottleneck in the immune response, which we can block effectively."
Antibiotic-resistant staphylococcus and streptococcus infections can cause sepsis, toxic shock, pneumonia, and post-surgical infections, and due to their multi-drug resistance, scientists have many problems with effective antibiotic development.
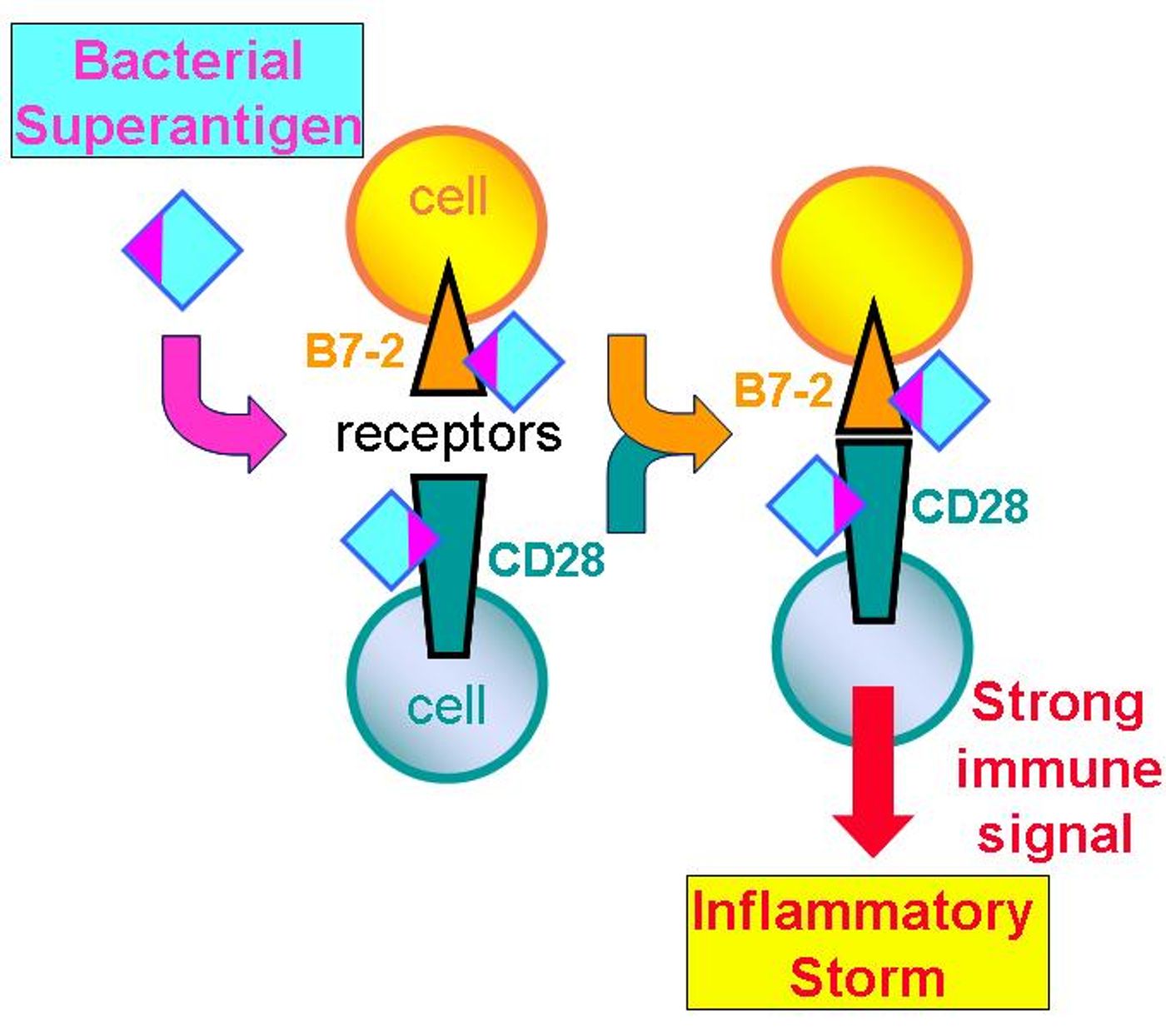
The bacteria incorporate superantigens, virulence factors that are highly lethal to humans, to stimulate what scientists are calling the “immune storm,” an overactive immune response that turns inflammation from a protective mechanism into a harmful action. The immune storm caused by these bacterial toxins can lead to multiple organ failure, a condition exacerbated by the fact that the infections are untreatable by most antibiotics.
Kaempfer’s recent study focused on a specific mechanism of the antigen-mediated immune response: the binding of superantigens to surface receptors, a process facilitated by so-called “costimulatory” receptors. They found that superantigen binding, as opposed to normal antigen binding, involved the simultaneous binding of two receptors at once: B7-2 and CD28, the beginning of the “receptor bottleneck” Kaempfer described.
The direct binding of both the costimulatory receptors enhances the binding interaction and is responsible for the hyperactivation of T cells that causes the immune storm.
In the study, the researchers looked at the potential of antagonists they designed to block the action of bacterial toxins in order to prevent infection, using a “novel, host-oriented therapeutic approach.” They designed peptides containing pieces of the human B7-2 receptor protein that blocked the binding of superantigens to the costimulatory receptor targets, showing in animal models that they protected against toxic shock.
"The strategy of using peptides that mimic regions of a human immune receptor, to put the brakes on the excessive inflammatory response triggered by superantigen toxins, is a host-oriented strategy that is broadly effective against the diverse family of superantigens," said Prof. Raymond Kaempfer.
The study was recently published in the journal
Proceedings of the National Academy of Sciences.
Sources:
The Hebrew University of Jerusalem