Stopping Inflammation Early to Prevent Blindness From Macular Degeneration
Macular degeneration is considered to be an incurable eye disease, but a new discovery from University of Virginia scientists may change that. A new study, published in Nature Medicine, identifies a specific enzyme involved in the immune response that has also surprising role in sparking inflammation that leads to blindness for the 200 million people living with macular degeneration worldwide.
"For the first time, we know in macular degeneration what is one of the very first events that triggers the system to get alarmed,” explained UVA’s Jayakrishna Ambati, MD. “This overdrive of inflammation is what ultimately damages cells, and so, potentially, we have a way of interfering very early in the process."
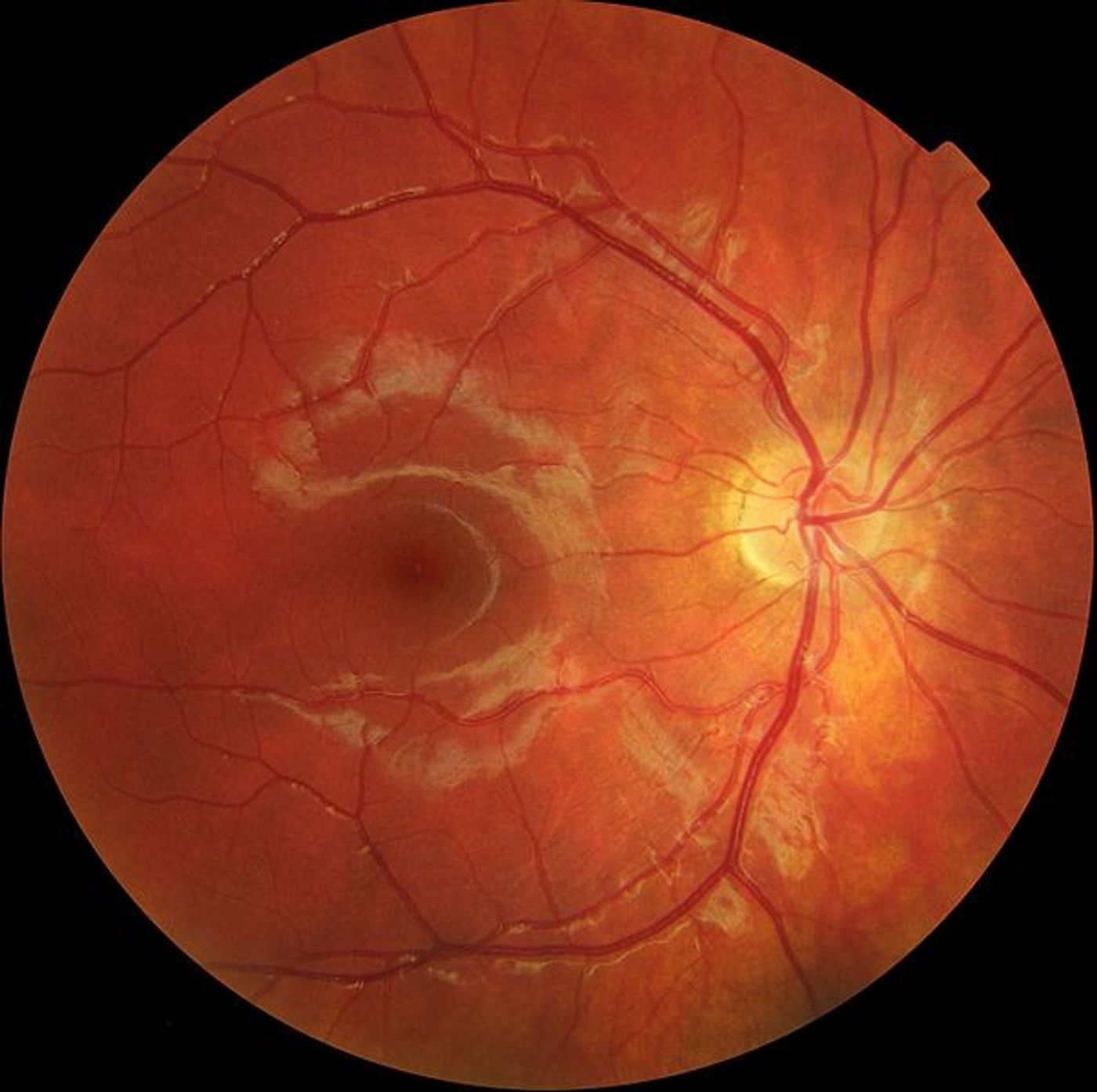
Macular degeneration, more than glaucoma and cataracts combined, is the leading cause of blindness among the elderly. It is caused by the deterioration of the central portion of the retina, called the macula, which provides vision we use to read, drive, and recognize faces.
A large majority of macular degeneration cases are of the “dry” type, which means that small deposits that form on the retina are responsible for deterioration. However, 10-15 percent of cases are the “wet” type, which means that deterioration occurs more quickly and more severely. Deterioration in cases of wet macular degeneration is caused by abnormal blood vessels that grow under the retina and toward the macula, which tend to break, bleed, and leak fluid. Little is known about what causes macular degeneration other than that it is a mix between genetics and environment.
However, the newest discovery of the involvement of an enzyme called cGAS provides an exciting opportunity for medical intervention: reducing inflammation to prevent blindness.
Past studies recorded the role of cGAS in the immune response to infections - the enzyme detects foreign DNA. But when scientists recently discovered that cGAS also plays a part in dry macular degeneration, they were surprised, because no research has ever suggested that macular degeneration is connected to invading bacteria or viruses.
Nonetheless, cGAS is indeed activated during the development of this form of the disease, and its activation alerts the immune system and results in retinal cell death and, ultimately, vision loss. These findings suggest that cGAS might also be potentially connected to other diseases related to the immune system, including diabetes, lupus, and obesity.
With cGAS identified as a target for treating macular degeneration, the clear next step is to drug development based on stopping cGAS from functioning in the context of macular degeneration, but the process will take several years to complete, as comprehensive tests for safety and efficacy are needed. Researchers are also interested in designing clinical tests to measure cGAS levels in the eyes of patients with macular degeneration, to help identify most at-risk candidates for a potential cGAS-inhibiting drug.
"Because the target we're talking about is an enzyme, we could develop small molecules that could block it," explained Nagaraj Kerur, PhD. "There are many drugs already on the market that target specific enzymes.”
Sources: American Foundation for the Blind, American Macular Degeneration Foundation, University of Virginia Health System