Potential Treatment ID'ed for Emerging Viral Disease
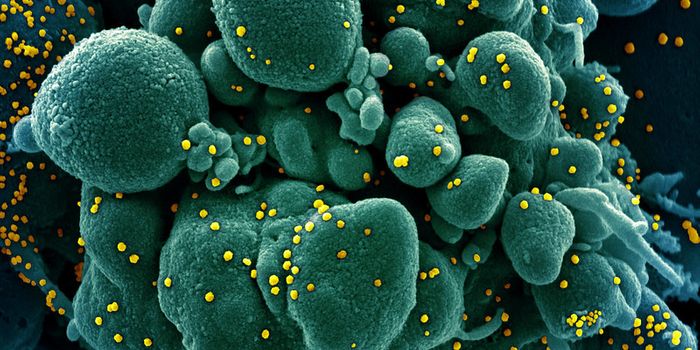
A mosquito-borne virus called Venezuelan equine encephalitis virus (VEEV) has been emerging in South America. It causes symptoms that make it difficult to distinguish from other diseases that are common in the area like dengue, and because it is tough to identify without sophisticated laboratory tests, it may be more common than we know. Climate change may also cause the disease to spread to other areas.
Scientists have now identified a molecule that might help create a treatment for VEEV. Reporting in Nature, the researchers found that this compound was able to protect mice from these viral brain infections.
"This virus can infect many species of wild mammals, and every few years it jumps from animals to humans via mosquitoes and causes thousands of infections and many deaths," said senior study author Michael S. Diamond, MD, Ph.D., the Herbert S. Gasser Professor of Medicine and a professor of molecular microbiology, and of pathology and immunology at Washington State University School of Medicine. "There's concern that with global warming and population growth, we'll get more outbreaks."
When mosquitoes transmit the virus to humans, it goes after neurons. When the virus infects these cells, it causes symptoms like nausea, fatigue, muscle pain, vomiting, fever, and headaches. In serious cases, the virus penetrates the blood-brain barrier and causes encephalitis: inflammation in the brain that can be fatal.
For this work, the researchers had to first create a form of the virus that they could easily use in the lab. Because VEEV is only available to labs with high-security levels, they utilized a related virus called Sindbis virus and exchanged some of its genes with VEEV genes. They used the hybrid, called Sindbis-VEEV, to look for the protein it uses to enter host cells, and how to prevent that from happening.
The researchers applied the CRISPR gene-editing tool to delete mouse neuronal genes until identifying one whose absence stopped Sindbis-VEEV from entering cells. They found Ldlrad3, a gene that codes for a surface protein. The human and mouse versions of Ldlrad3 are similar, and when the human version was removed from various cell lines, Sindbis-VEEV infection was prevented. The opposite was also true; infection was enabled when the Ldlrad3 gene was added to cells that normally lack it. These findings were also replicated in a lab that was able to work with VEEV.
The scientists used a portion of the Ldlrad3 protein to make a kind of decoy for the virus to latch onto. Any virus that was bound to this decoy would be unavailable to infect cells. They tested the decoy they created in mice that were exposed to VEEV in a model of a mosquito bite as well as direct injection into the brain. Except for two of the ten mice that got direct brain exposure, mice that also got the decoy survived.
"In an outbreak situation, you may be able to use a drug like this as a countermeasure to prevent transmission and further spread," Diamond suggested.
Since a drug based on this molecule would mimic a human protein instead of a viral one, it's also less likely that the virus would develop resistance, the researchers noted.
A similar virus, Eastern equine encephalitis, has also been on the rise in the United States. Learn more from the video.
Sources: AAAS/Eurekalert! via Washington University School of Medicine, Nature