Epstein-Barr virus and cancer
Spoiler alert, you’re infected with Epstein-Barr virus. Well, you’re probably infected - nearly 98% of people are.
EBV is a herpes virus (human herpes virus 4, to be exact). Most people who get EBV don’t even experience symptoms. In adolescents, however, the virus causes mononucleiosis about 30-50% of the time. Symptoms include fever, sore throat, swollen lymph nodes, rash, and an enlarged spleen and liver.
More importantly, EBV can cause cancer. It is associated with cases of Hodgkin’s lymphoma, Burkitt’s lymphoma, and gastric and nasopharyngeal cancers. As for most viruses, people with compromised immune systems are especially susceptible - EBV causes hairy leukoplakia and lymphoma in people with HIV.
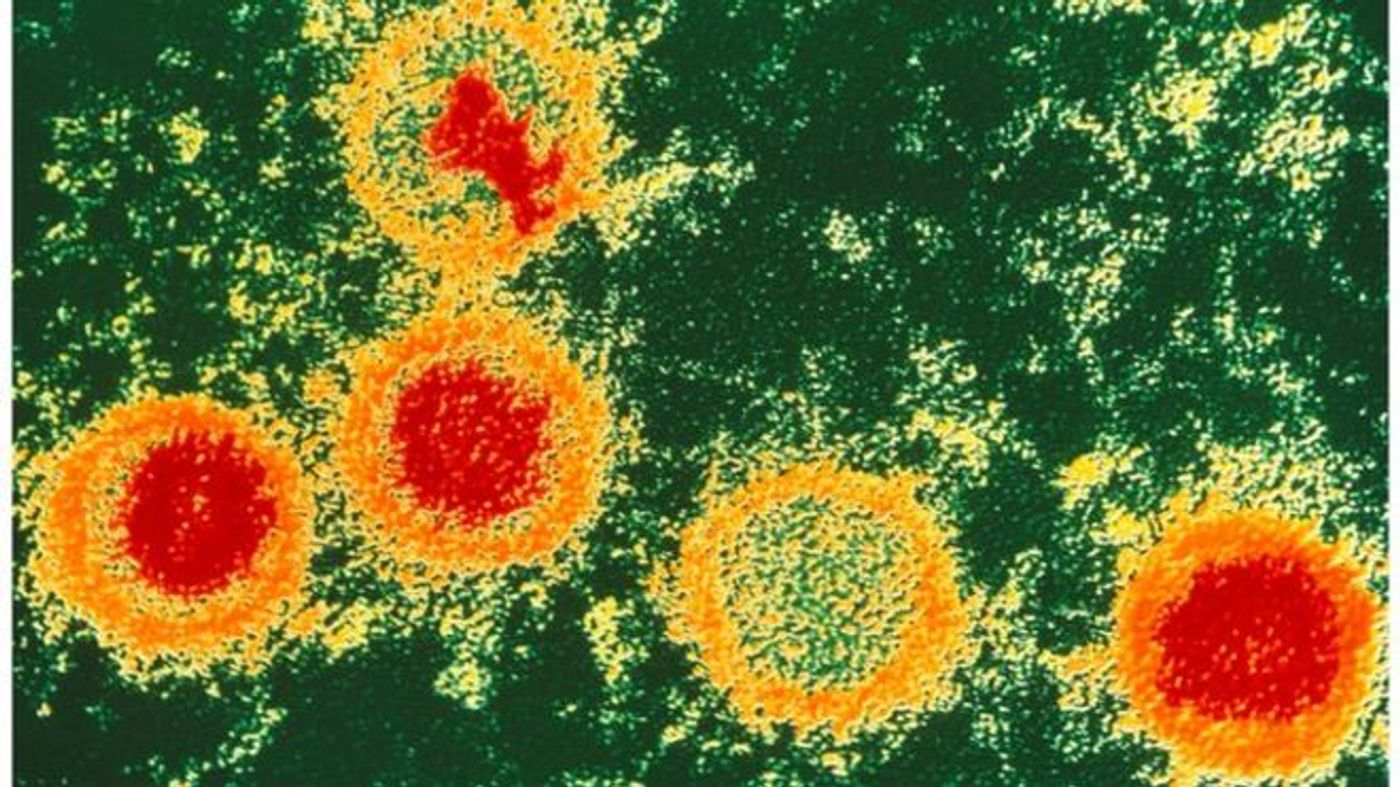
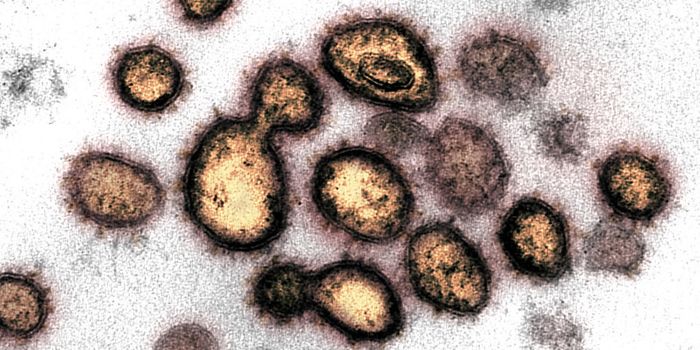
EBV, like all herpes viruses, is shaped like an icosahedron - it has 20 triangular sides. This icosahedral capsid surrounds the double-stranded viral DNA and is itself surrounded by an envelope. This envelope contains host cell proteins from the nuclear envelope and endoplamsic reticulum that it picks up during its life cycle in the host cell.
EBV infects epithelial cells and B cells. Like all herpes viruses, it has two life stages - and active and latent stage. In the active, or lytic, phase, EBV replicates to produce more viruses. During the latent stage, however, the virus incorporates its DNA into the host cell’s DNA.
EBV causes cancer by immortalizing (or “transforming”) B cells - it prevents apoptosis and encourages cell division. In most cases, the immune system destroys these immortalized cells, but that’s not the case for immunocompromised individuals.
Transformation requires EBV to express LMP1 and EBNA family proteins. LMP1 is probably the best-studied EBV latent protein and contributes to B cell proliferation. During latency, LMP1 is expressed on the membrane of infected B cells where it mimics CD40, the tumor necrosis factor receptor.
Early research into LMP1 showed that cell lines expressing LMP1 proliferated readily, and these cells caused tumors when injected into immunocompromised mice. If B cells expressed a mutant version of LMP1, however, the cells proliferated normally - if a wild type copy of the gene was restored, the cells proliferated uncontrollably.
How exactly does LMP1 induce proliferation? One way is by upregulating NF-κB. This factor has a number of cellular functions, but one is establishing inflammation-associated tumor growth. LMP1 upregulates NF-κB signaling by interacting with TRAFs - tumor necrosis factor receptor-associated proteins. In one scenario, LMP1-activated TRAFs may recruit the host protein NIK (NF-κB-inducing kinase). NIK phosphorylates IKKα, which then phosphorylates IκBα. This causes IκBα, which normally inhibits NF-κB, to be degraded. Thus, NF-κB can enter the nucleus and act as a transcription factor, presumably driving cell proliferation.
Not all cases of transformation require LMP1, however - LMP1-mutant viruses can still transform cells, although with very low efficiency. This means that other factors also promote EBV-mediated host cell transformation.
Just this week, researchers in Germany revealed a new mechanism by which the EBV protein BNFR1 alters host cells, possibly leading to cancer. For example, they found that EBV replication increases chromosome instability in B cells. Specifically, EBV infection causes chromosomes to organize abnormally during mitosis in 15-42% of cells, and up to 7% of cells formed more than four centrioles during division. As infection progressed, the researchers observed aneuploidy in up to 40% of cells, with around 3% being polyploid.
According to study author Henri-Jacque Delecluse, “the novelty of our work is that we have uncovered a component of the viral particle as a cancer driver. All human tumor viruses that have been studied so far cause cancer in a completely different manner. Usually, the genetic material of the viruses needs to be permanently present in the infected cell, thus causing the activation of one or several viral genes that cause cancer development. However, these gene products are not present in the infectious particle itself."
While there’s plenty of evidence that EBV causes cancer, there are also many reported cases of EBV-negative Hodgkin and Burkitt lymphomas. In these cases, researchers think that EBV may be present in the original tumor clone, but is lost as the tumor cells proliferate. Alternately, these cancers may be caused by other genetic mutations - mutations that have the same effects as EBV infection.
Sources: Science Daily, MicrobeWiki, Nature Communications, Nature Reviews Immunology, Wikipedia