Proposed New Criteria For Diagnosing Parkinson's
A new review published in the Journal of Parkinson’s Disease suggests that our previous diagnostic criteria for Parkinson's Disease (PD) is inadequate and should be revised. This revised criteria would involve examining patients for prodromal symptoms associated with the disease. Prodromal symptoms are symptoms that are non-PD-like but have a high rate of occurrence in individuals that go on to develop PD. Earlier detection of these symptoms could promote earlier treatment and better outcomes.
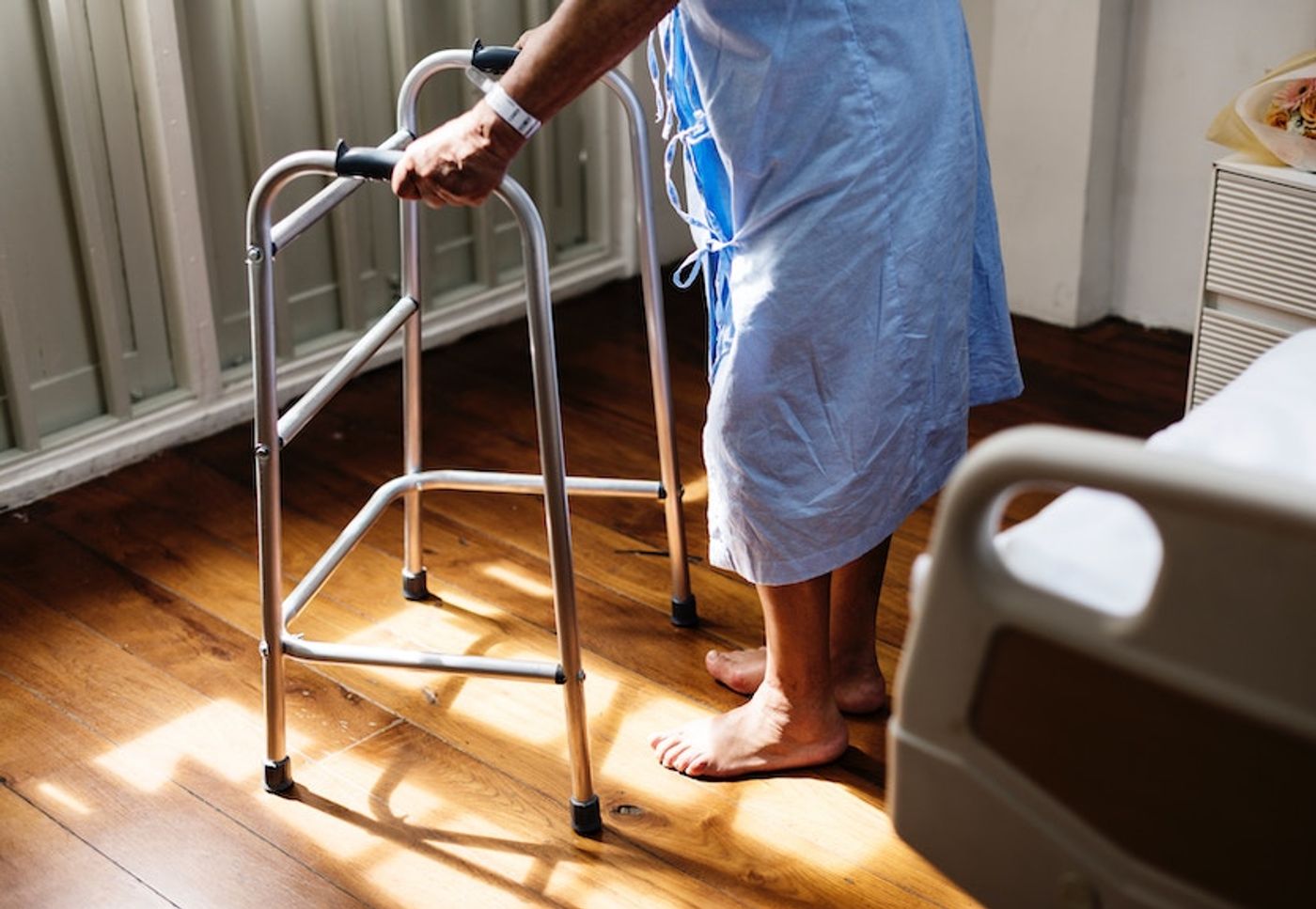
Photo source: UnSplash.com
What constitutes prodromal symptoms have been debated, however, the typical symptoms of prodromal PD are mood disorders, autonomic disturbances, cognitive impairment, and sleep disturbances. Other symptoms that have been shown to correlate with a future diagnosis of PD are hyposmia, constipation, and idiopathic REM Sleep Disorder. These symptoms present themselves before the classic motor symptoms that are currently used to diagnose PD (bradykinesia, tremor, rigidity, and postural instability).
The authors of the present review suggest that prodromal PD can last as long as years to decades. This, according to the authors Drs. Daniela Berg, MD, of the Christian-Albrechts-University of Kiel, Germany, and Ronald B. Postuma, MD, MSc, of Montreal General Hospital, suggests that non-motor and subtle motor symptoms may indicate a slow spreading PD pathology. Essentially, PD may not start at the level of the substantia nigra but spread to this area during the prodromal phase. Unfortunately, even the classical motor-based diagnosis is not definitive. To get an absolute diagnosis of PD one has to confirm it with an autopsy.
The authors of the review advocate a new system of diagnostics, which includes an acceptance that prodromal symptoms are actually signs of PD. They also recommend a closer look at the increasing data pointing to certain risk factors and correlate them to imaging and histopathological findings. Finally, they implore for more longitudinal studies that observe conversion to PD in cohorts of individuals with different combinations of risk and prodromal markers. The main idea is to find more diagnostic criteria and link it to current imaging methods to find where in the brain certain changes are taking place. Furthermore, their goal is to screen for legitimate prodromal symptoms so that they can be addressed in the clinician's office.
Photo source: UnSplash.com
Prodromal symptoms are not the same as pre-clinical symptoms for PD. Pre-clinical refers to a stage where no PD-related symptoms are present and the diagnosis of PD has not been declared. The prodromal period, however, begins before the loss of dopamine cells in the substantia nigra that are necessary for movement. This suggests that PD is a slowly spreading neurological disease which may even start outside of the brain. The gut has been suggested as a candidate. The olfactory system may also play a role. Essential, PD may start elsewhere and slowly encompass much of the nervous system.
Thus, if clinicians and scientists accept legitimate prodromal symptoms to diagnose PD, this will lead to earlier detection and earlier treatment. Yet, in doing so, they will have to accept the idea of PD as a slowly progressive neurological disorder with a possible etiology outside of the brain, if not just the substantia nigra. The concept of PD as a motor-disorder, and waiting for the motor symptoms to arise, could shave off years of treatment to either halt the progression of the disease or slow it down. It may be time to start looking for earlier warning signs.
Here is a video from Dr. Wolfgang H. Oertel, MD, Ph.D. from the University of Marburg, Marburg, Germany with further explanation.
Sources: Journal of Parkinson’s Disease, Movement Disorders, European Journal of Neurology, https://en.wikipedia.org/wiki/Hyposmia, Journal of Neurology