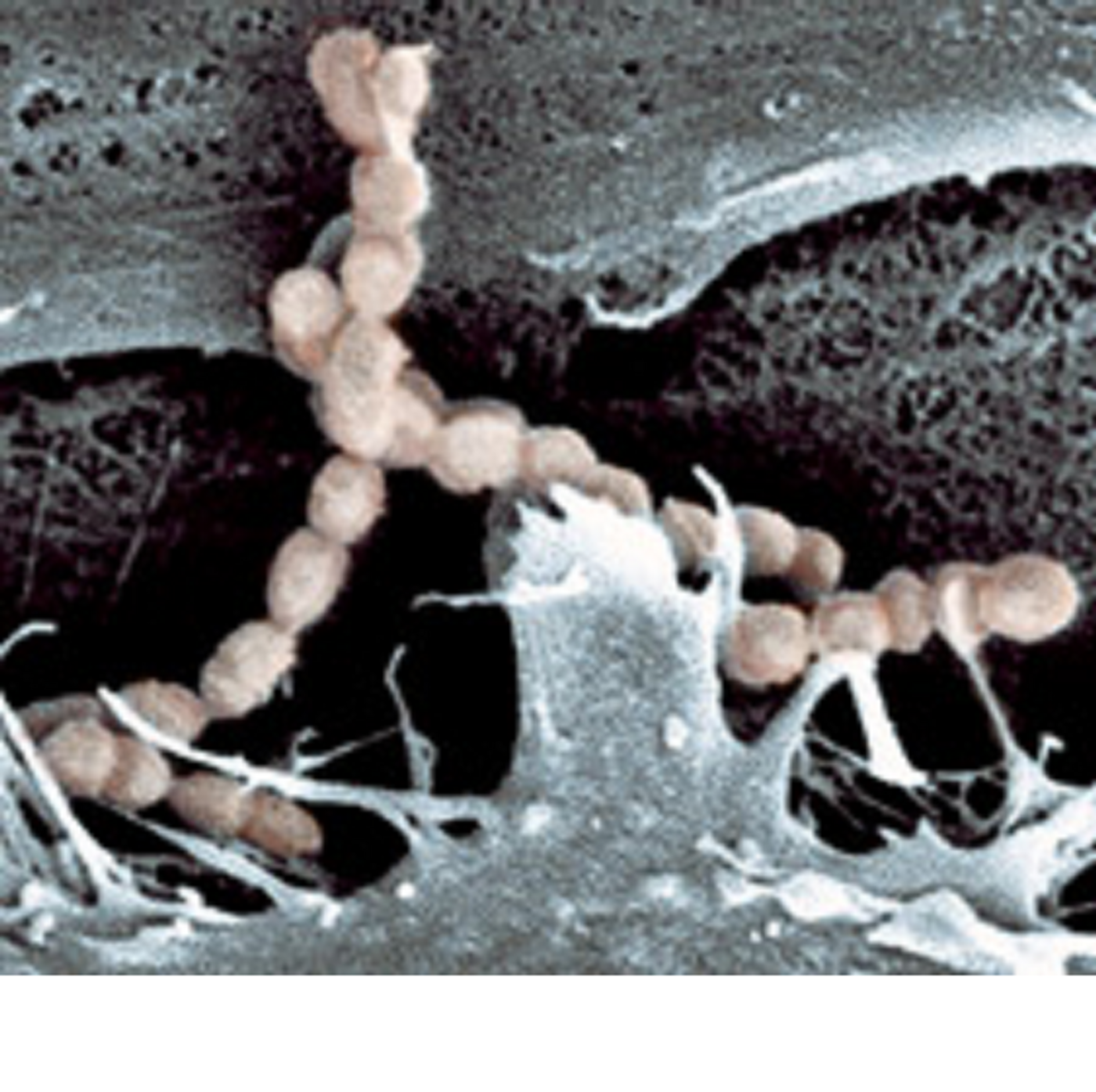
Streptococcus suis is a swine pathogen that was first reported in 1954 and is responsible for severe economic losses in the swine production industry. Infection in swine leads to meningitis, septicemia and arthritis in piglets.
S. suis is now considered an emerging pathogen in humans with the first cases in humans identified in the 1960s in Denmark and Hong Kong. It has been identified as the third most common cause of adult meningitis in Hong Kong and the second cause of meningitis in Vietnam and Thailand with greater than 700 cases per year occurring globally. Scientists speculate that the emergence of
S. suis in humans is due to increased capacity to infect humans in certain geographical areas as well as the increased awareness and improved detection of
S. suis in humans.
A previous study showed that 63% of patients infected with
S. suis experiencing symptoms of “Streptococcal toxic-shock-like syndrome (STSLS)” presented high serum levels of IFN-γ, TNA-α, IL-8, IL-12 and IL-1β. Similar studies in mice showed that experimental infection to induce STSLS led to increased levels of pro-inflammatory cytokines which seemed to play a role in the development of meningitis and sudden death.
More recently, it was confirmed that the triggering receptor expressed on myeloid cells-1 (TREM1) gene appeared to boost the immune response and played a role in the clearance of
S. suis during infection. Researchers from Huazhong Agricultural University in China aimed to determine whether the introduction of recombinant TREM1 could be used to inhibit the signaling of immune cells in the presence of antibiotic resistance. They also sought to evaluate the role of TREM1 in the immune response related to STSLS caused by
S. suis and whether or not TREM1 could be used to boost clearance of bacteria in the presence of antibiotics.
According to the article published in
Frontiers in Cellular Infection Microbiology, authors found that rTREM1 “aggravated”
S. situ infection in a mouse animal model. In their control experiment, they treated mice with antibiotics only (no rTREM1) and found that the rate of survival in mice did not increase following the treatment. In contrast, combined treatment with rTREM1 and antibiotics led to proficient bacterial clearance as well as alleviated inflammation. These effects were due to the reduction of the exaggerated pro-inflammatory response in mice caused by rTREM1. The authors concluded that blockage of TREM1 signaling could be an effective target in the treatment of STSLS in the presence of antibiotics.
Sources:
Frontiers in Cellular and Infection Microbiology;
Clinical Infectious Diseases