New Insight Into An Old Bacterial Pathogen
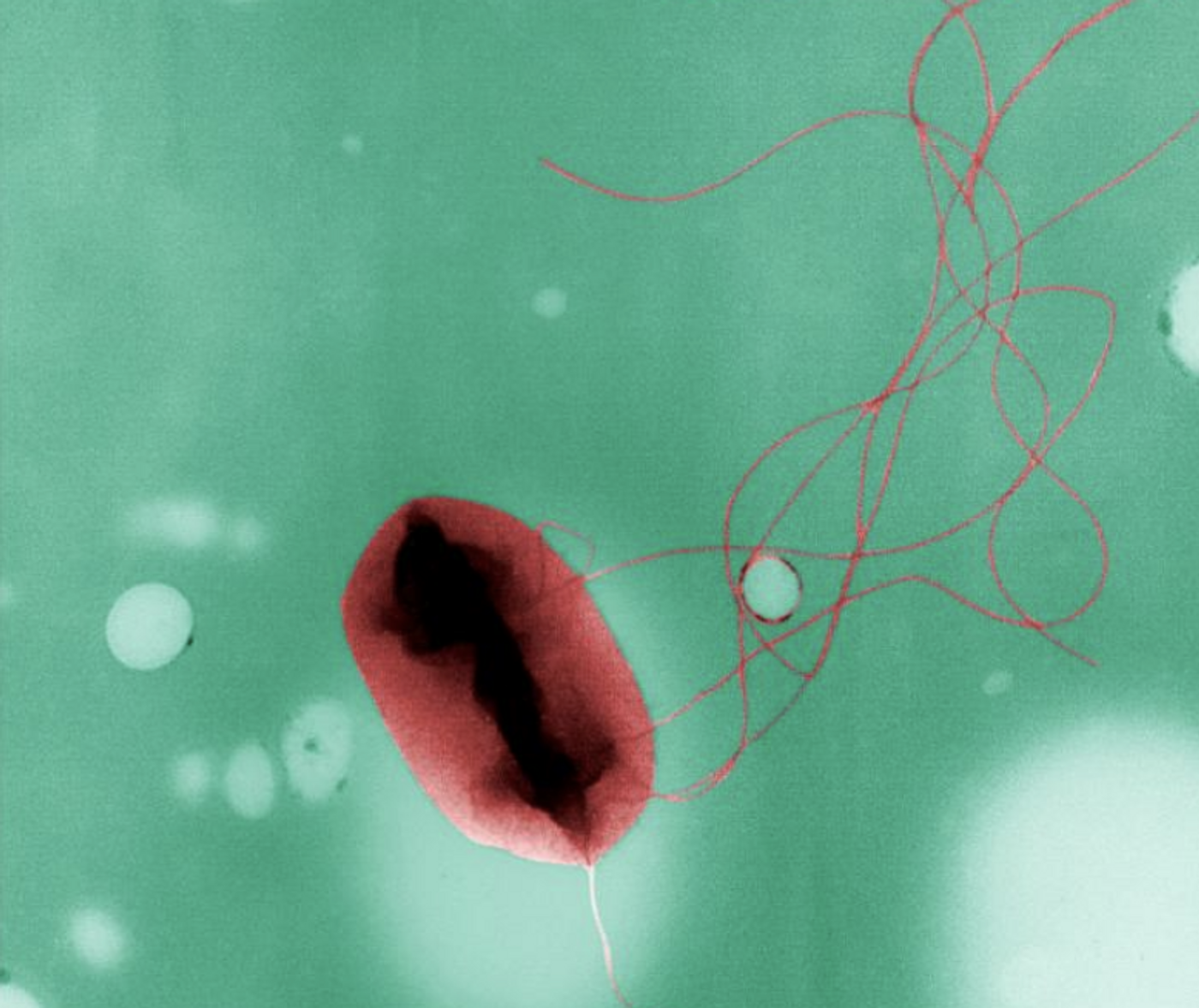
There are many different strains of Escherichia coli bacteria, some of which live harmlessly in the human gut. But some E. coli strains, like enterohemorrhagic E. coli (EHEC), can cause serious gastrointestinal illness. These microbial pathogens produce a dangerous toxin called Shiga, which can go on to damage the kidney and nervous system. Scientists have now identified a biochemical pathway that leads to the production of these toxins.
The findings, which have been reported in the Proceedings of the National Academy of Sciences (PNAS), may help scientists create a treatment for these gastrointestinal infections; currently there is none.
"Antibiotic treatment of these infections is generally not recommended because antibiotics stimulate production of the Shiga toxin, leading to an increased risk of kidney failure, neurological damage, and death," explained the senior author of the study, Dr. Jai Tree. "The new pathway that we have found reduces toxin production and is not expected to be stimulated by antibiotic treatment. So, our results identify a potential new target for the development of drugs that can suppress Shiga toxin production during EHEC infection.
Much more work must be done before that treatment is created, Dr. Tree acknowledged. "It's still early days, however, and we need to conduct a lot more research to understand if our findings apply to a broad range of clinical EHEC isolates and to both types of Shiga toxins produced by human EHEC isolates."
While people may come into contact with EHEC because they are in close proximity to farm animals and their feces, or trace amounts of feces from an infected person, people can also be exposed by eating EHEC-contaminated food that has not been properly cooked, or uncooked food that has been contaminated with fecal matter.
"Children under five years old and older people are at greatest risk of developing an EHEC infection," noted Dr. Tree.
Although EHEC infections don’t cause as much illness as other foodborne pathogens, the illness can be very serious or fatal, he noted.
"EHEC outbreaks occur sporadically in Australia and worldwide. The most significant outbreak occurred in South Australia in 1995 and was caused by contaminated mettwurst, a semi-dry fermented sausage made from raw minced pork preserved by curing and smoking," he said.
In 2011, there was also a large outbreak in Germany.
"The strain in Germany was spread mostly via consumption of contaminated sprouts and in several cases, from close contact with an infected person," he added. "During this outbreak, more than 4000 people were infected and 50 people died."
RNA sequencing enabled the researchers to identify non-coding RNA that was performing regulatory functions.
"We discovered a very short piece of the toxin messenger RNA is made into a regulatory non-coding RNA that silences the toxin and promotes growth of the pathogen,” said Tree. "This new regulatory non-coding RNA had been hiding in plain sight for almost 20 years," he added.
"Our work shows a new mechanism for controlling toxin production that may be amenable to new RNA-based therapeutics to inhibit toxin production during an infection. We anticipate this would expand intervention options and potentially allow use of antibiotics that are currently not recommended because they stimulate Shiga toxin production.
Sources: AAAS/Eurekalert! via University of New South Wales, Proceedings of the National Academy of Sciences