Bad News for Vegetarians: Antibiotic Resistant Bacteria Found in Produce
According to the World Health Organization (WHO), antibiotic resistant microorganisms such as bacteria, viruses, fungi and parasites, have the developed as a result of over exposure to antimicrobial drugs such as antibiotics, antifungals, antivirals, antimalarials and antithelmintics.
Researchers have found lettuce and tomatoes purchased from grocery stores in China harbor Escherichia coli and Raoultella ornithinolytica that are resistant to the last resort antibiotic colistin. Credit: Thinkstock
These organisms are often referred to as "superbugs" because they can infect and persist within the host because the medicines previously used to kill these organisms are no longer effective. Antibiotic resistant organisms have begun to cause complications for cancer chemotherapies, diabetes management, major surgeries, and the fight against HIV. The cost of health care with lengthier hospital stays and time in intensive care has also become a concern.
As antibiotic resistance has begun to spread globally, it has become a top priority across all government sectors and society. National summary data reported by the Centers for Disease Control and Prevention (CDC) in 2013 estimated that there are a minimum of 2,049,442 illnesses and 23,000 deaths attributed to antibiotic resistance each year. It has been estimated that by the year 2050, antibiotic resistance will have resulted in approximately 300 million deaths.
While antibiotic resistance occurs naturally overtime, misuse and overuse of antimicrobials has accelerated this process. Antibiotic misuse can occur when antibiotics are prescribed to someone who does not have an infection or when they are used as growth promoters in animals. These "superbugs" are ubiquitous in nature and can be found in people, animals, food, water, soil, and air. These microbes are spread through the environment by poor infection control, inadequate sanitary conditions, and inappropriate food-handling.
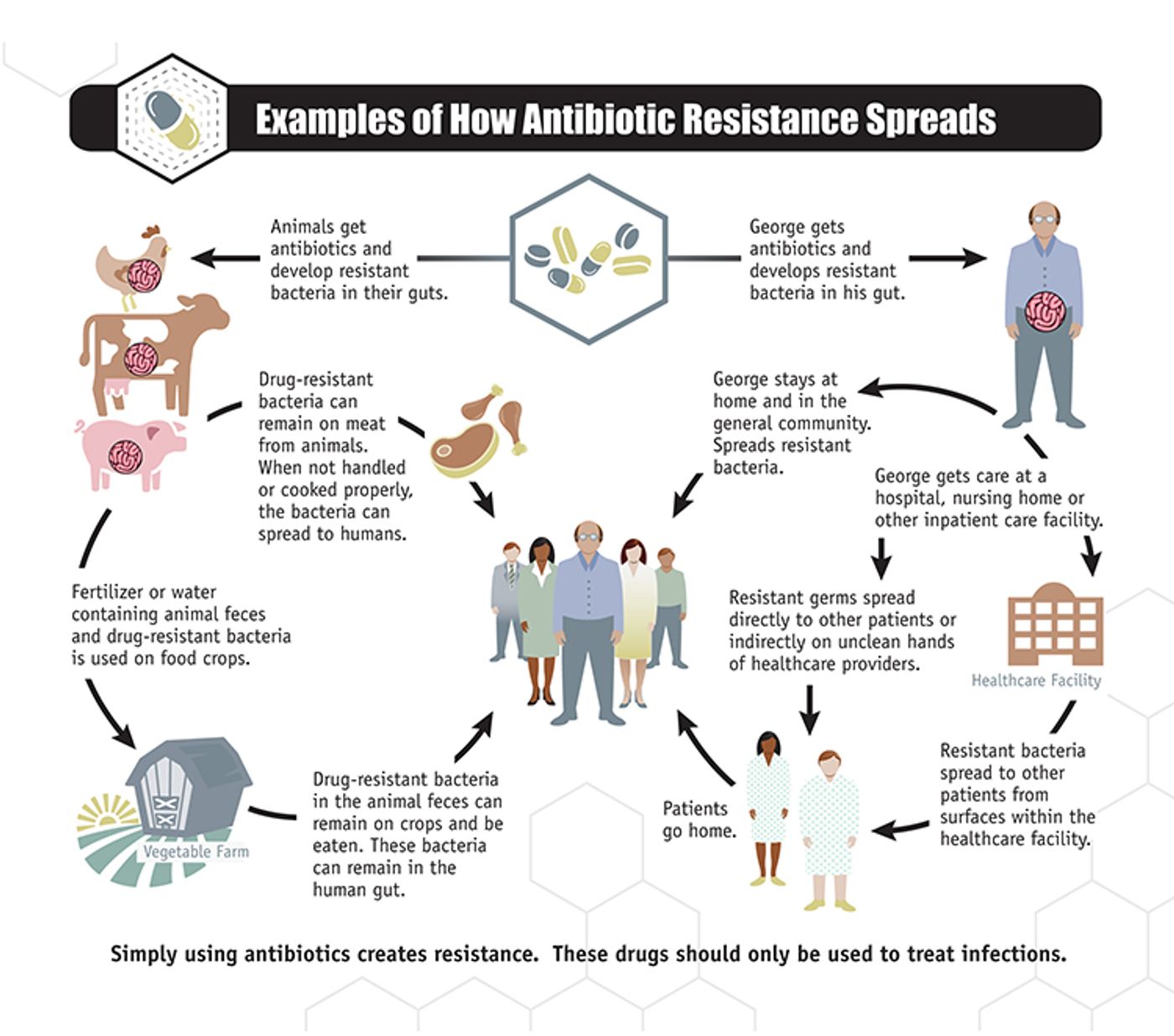
Antibiotic resistance can spread through the environment through direct person-to-person contact or through contact with animals or the ingestion of contaminated food. Credit: Centers for Disease Control and Prevention
Antibiotic resistance can occur in human medicine as well as veterinary medicine. In both cases, antibiotic resistance can develop in the gut after antibiotics have been consumed and shed in the feces. Antibiotics have been used widely in animal production since the 1950s and 1960s and have provided significant benefits including faster weaning times, higher animal densities, cheaper feed prices, increased outputs, and cheaper cost of meat. Despite these benefits, as a society we are now experiencing the consequences of the misuse of antibiotics in animal production including a serious public health threat. Other consequences include ecological imbalance, multi-drug resistance and cross-resistance, spread of resistance to other pathogens, and zoonotic transmission.
While transmission can occur through direct contact with other humans or animals, transmission can also occur through the ingestion of contaminated food. According to the Food and Agriculture Organization (FAO), the major route of transmission pathway for resistant bacteria and resistance genes is from food animals to humans. It now appears that antibiotic resistance can also be spread through edible plants including fresh vegetables. According to an article published in the current issue of Antimicrobial Agents and Chemotherapy, researchers from South China Agricultural University in Guangdong, China and the University of Pittsburgh Medical Center in Pittsburgh, PA reported that they isolated two Raoultella ornithinolytica and seven Escherichia coli strains from lettuce and tomato samples that were found to harbor the mcr-1 gene, which confers resistance to the "last resort" antibiotic known as colistin.
Between May 2015 and August 2016, the authors of this study collected 916 fresh vegetable samples from local supermarkets in Guangzhou, China. From these samples, 244 antibiotic resistant ESBL-producing bacteria were recovered. Of those 244 isolates, 6 (2.5%) were found to be positive for mcr-1. Prevalence of mcr-1 in ESBL-producing E. coli isolates was higher than that of other bacterial species found in vegetables samples (17.4%). Four of the ESBL-producing isolates were found to be resistant to colistin but were negative for both the mcr-1 and mcr-2 genes. All nine of the isolates carrying the mcr-1 gene demonstrated resistance to both colistin and florfenicol. Use of pulsed field gel electrophoresis (PFGE) and multilocus sequence type (MLST) analysis revealed that some of the mcr-1-positive isolates were genetically related.
The authors conclude that although the occurrence of mcr-1 isolates from vegetables is lower than that of isolates found in food animals, the presence of mcr-1-producing bacteria in vegetables presents a threat to human health especially because fresh vegetables are most often consumed in the raw state. The presence of mcr-1-positive organisms in the food supply is alarming and authors suggest appropriate measures should be taken in order to improve food safety and consumer health. Proper disposal and/or treatment of animal waste before being applied as a fertilizer on food crops and improvement of the quality of irrigation water should be considered. Further studies are needed in order to better asses the risks associated with the spread of antibiotic resistance through the consumption of fresh fruits and vegetables.
Sources: Antimicrobial Agents and Chemotherapy, Centers for Disease Control and Prevention, World Health Organization, Food and Agriculture Organization