Treatment Strategies for Multidrug-resistant Chronic Infections
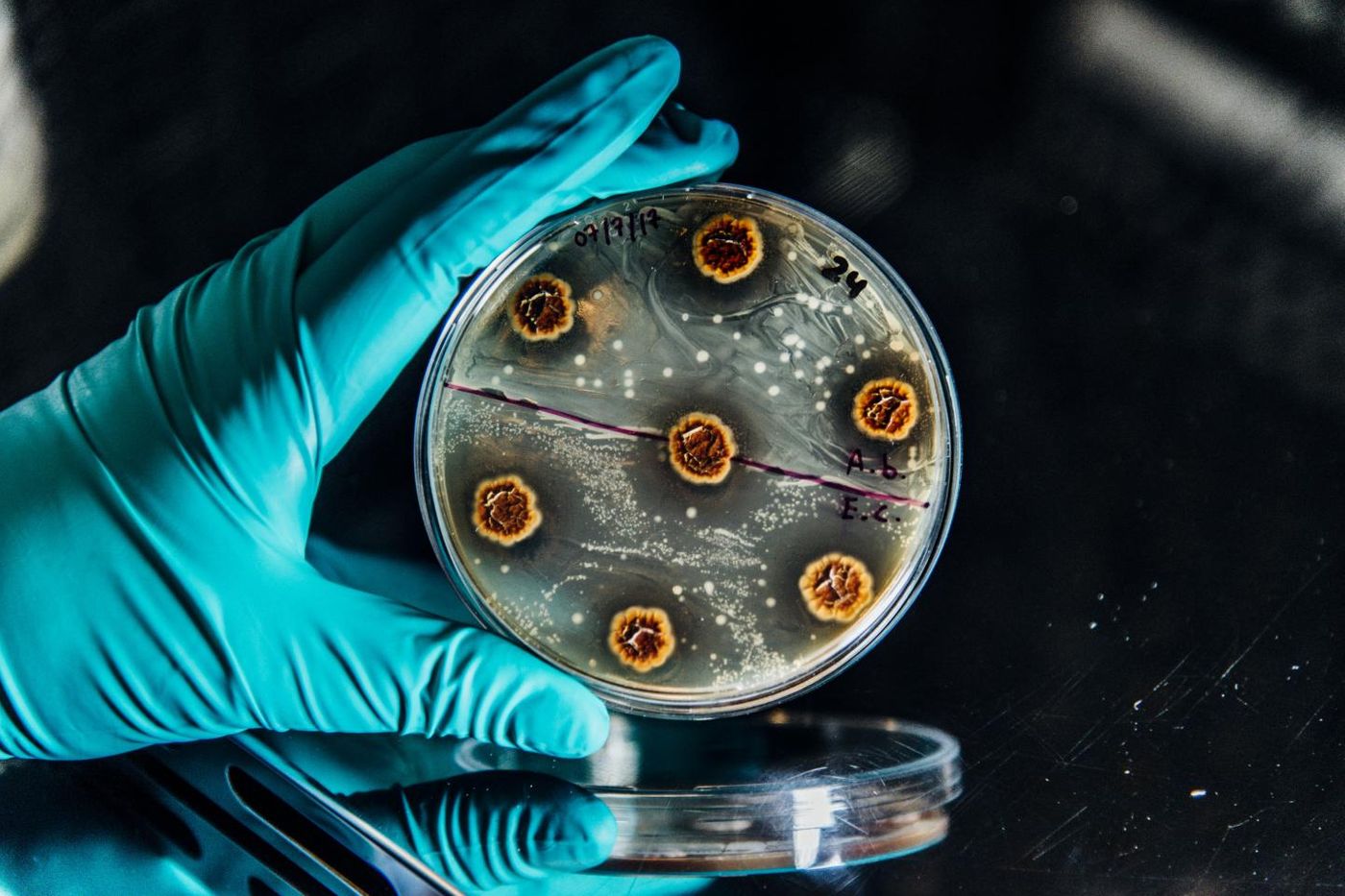
Cystic-fibrosis (CF) patients have enough problems, by they are also often plagued by antibiotic-resistant infections with Pseudomonas bacteria. These infections are apparently susceptible to certain classes of antibiotics. A new study reported in Cell by researchers at the Novo Nordisk Foundation Center for Biosustainability of the Technical University of Denmark suggested that this work may help doctors optimize the treatment of chronic infections for individual patients.
"Our discovery of widespread antibiotic sensitivities in the multidrug-resistant pathogen Pseudomonas aeruginosa opens up the opportunity to limit the development of antibiotic resistance and perhaps even revert it. This could be important for the treatment of several chronic infections including the life-long lung infections of patients with cystic fibrosis," noted Morten Sommer, Professor and Scientific Director at the Novo Nordisk Foundation Center for Biosustainability.
The scientists discovered that some vulnerabilities to antibiotics are maintained in multidrug-resistant pathogens across clinical isolates obtained over many years at the Cystic fibrosis clinic in Rigshospitalet in Copenhagen. The analysis revealed the mutations that caused these sensitivities, as well.
"Targeting vulnerabilities of phenotypic states related to specific mutations could potentially have a huge impact because it makes it possible to make a more personalized treatment strategy for each patient,” explained Lejla Imamovic, Senior Researcher at the Novo Nordisk Foundation Center for Biosustainability.
"Results indicate that for some antibiotics, exposure and subsequent resistance evolution leads to convergence toward specific phenotypes states. Thus, collateral sensitivity may be particularly useful for optimizing treatments of chronic infections since their nature and severity warrants and requires tailored treatment strategies," said Lejla Imamovic.
Scientific knowledge is one thing, but usefulness in the clinic is another. Currently, it is thought that pathogens evolve, becoming increasingly resistant in response to antibiotic treatment, causing a chronic infection. However, widespread collateral sensitivity interactions suggest that chronically infectious bacteria have fluctuating resistance profiles in response to different drugs, according to Sommer.
"Our research supports the notion that treatment of chronically infected patients could be significantly improved based on specific diagnostic markers that are associated with a collateral sensitivity to specific drugs," he said. Now, the findings have to be applied to the patient.
"Actually, some of our findings relate to drugs that are already used clinically and it is possible that benefits can be gained simply by making slight changes to the empirical treatment prescribed by physicians already now. Yet, larger controlled clinical trials will also be important in order to fully exploit these findings in the clinic," noted Morten Sommer.
Learn more about Pseudomonas infections in CF from this video.
Soucres: AAAS/Eurekalert! Via Technical University of Denmark, Cell