Gene Therapy Saves a Butterfly Child
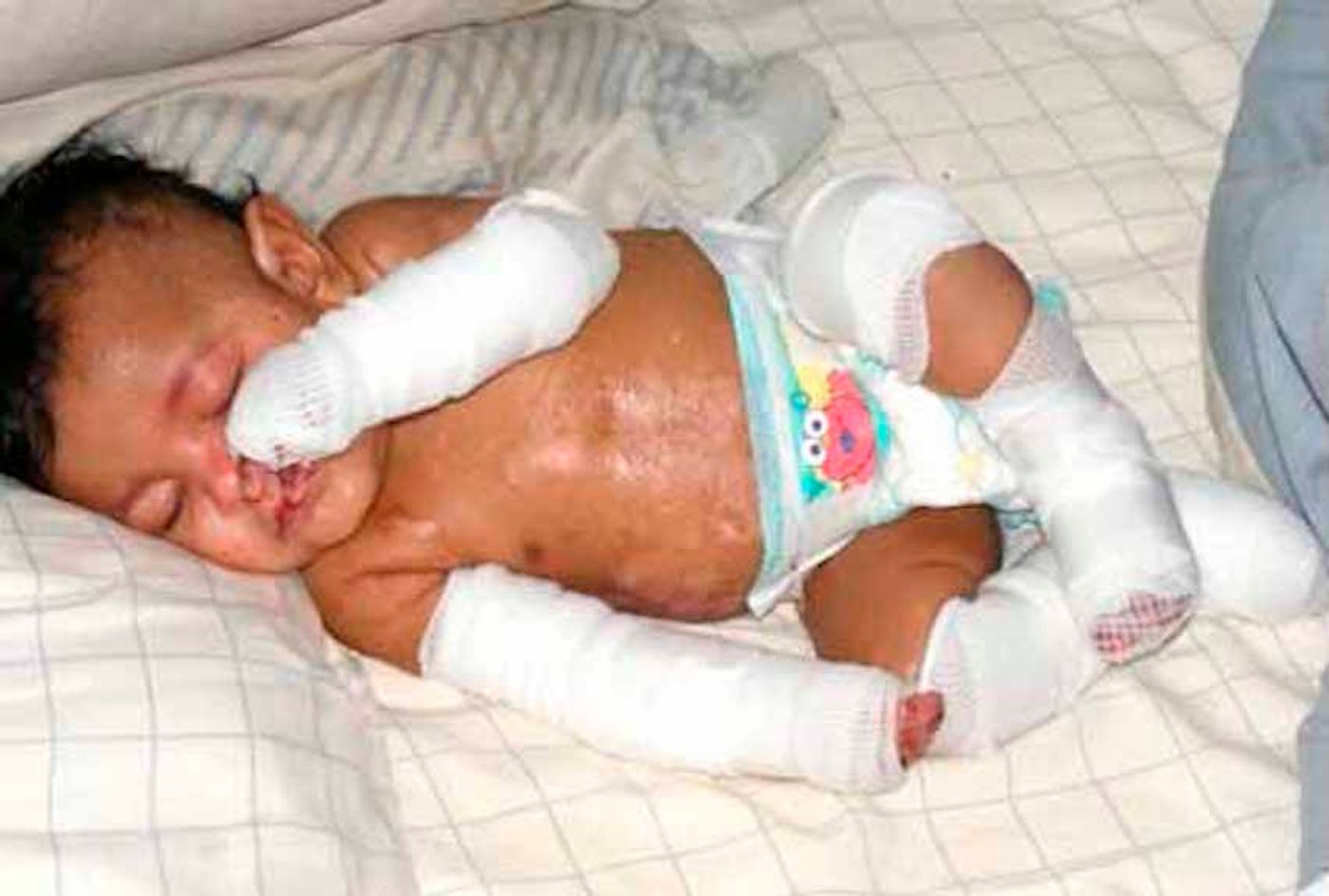
Children that suffer from epidermolysis bullosa, sometimes called butterfly children because of their fragile skin, face incredible challenges. The devastating genetic disease impairs skin regeneration; even minor stresses on the skin can cause wounds, blisters and skin loss, resulting in scarring. If the patient’s internal organs are also affected, it can be life-threatening. Scientists have now reported the successful treatment of an affected child, using transplants made from genetically altered stem cells. It has been two years since the start of his treatment, and the boy can now participate more actively in family and social functions. The research team from Ruhr-Universität Bochum's burn unit and the Center for Regenerative Medicine at the University of Modena (Italy) have reported their work in Nature.
When this patient was first admitted to a pediatric intensive care unit in June 2015, 60 percent of his body was affected, and his life was in danger. Conventional treatments were failing. "He suffered from severe sepsis with high fever, and his body weight had dropped to a mere 17 kilograms - a life-threatening condition," Dr. Tobias Rothoeft, Consultant at the University Children's Hospital at Katholisches Klinikum Bochum. The disease would eventually affect 80 percent of the patient’s skin.
The terrible outlook for the boy prompted the team of pediatricians and plastic surgeons to go for an experimental approach. Stem cells were harvested from the patient through a skin biopsy. The researchers led by Professor Michele De Luca from the Center for Regenerative Medicine at the University of Modena altered epidermal stem cells with a retrovirus that can deliver a corrected version of the mutated gene that causes the child's disease. The modified stem cells that resulted from the procedure were made into transplants for the patient.
They were applied to the arms, legs, back, flanks, the stomach, neck, and face of the boy. "Overall, 0.94 square meters of transgenic epidermis were transplanted onto the young patient in order to cover all defects, accounting for 80 percent of his entire body surface," said Associate Professor Dr. Tobias Hirsch, head consultant at the department of plastic surgery.
The first transplantation happened in October 2015, and the patient has been improving ever since. The genetically modified stem cells have formed new skin, and the binding proteins that are impaired in the disease are now intact in the transplanted areas. The retroviral gene transfer has been stable, successfully integrating the correct gene into the genome of the stem cells. The patient was discharged in February 2016. The patient has even been able to attend school, as stress-resistant skin has formed.
This is the first time a patient has been treated with transgenic epidermal stem cell transplants on a large area. "This approach has enormous potential for research into and development of new therapies for the treatment of epidermolysis bullosa as well as other diseases and trauma causing large skin defects," said Tobias Hirsch.
The massive scale of the transplant is thought to make the case unique worldwide. "Transplanting 80 percent of the skin and providing intensive medical care to the patient over a period of eight months was extremely challenging," Tobias Rothoeft and Tobias Hirsch noted. "The close collaboration between the departments in Bochum and the University of Modena's expertise [has] been the key to success. This makes us very proud."
While this treatment is not curative and cannot help patients whose internal organs are impacted, this is a major step in the right direction. The researchers are continuing their efforts, working now towards a treatment for another type of this kind of disease, dystrophic EB.
Sources: AAAS/Eurekalert! via Ruhr-Universität Bochum, Science, Nature